Alert: Canvas Update: May 13, 2026
Canvas is currently stable and available to use. After cybersecurity events like this, there is an increase in phishing and smishing attempts. Our Canvas administrators will never text you or contact you from an external email address. Please review the latest communication for steps to keep your information secure.
Learn More
Neurotrauma & Critical Care Program of Excellence
 Neurotrauma describes
two complex conditions: acquired brain injury (ABI) and spinal cord injury (SCI). Both are life-changing and can lead to significant ongoing chronic conditions.
Neurotrauma describes
two complex conditions: acquired brain injury (ABI) and spinal cord injury (SCI). Both are life-changing and can lead to significant ongoing chronic conditions.
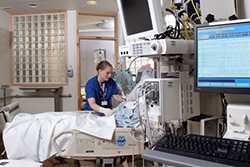 Acquired
brain injury can result in problems with attention, planning and interacting with others. Spinal cord injury can lead to permanent paralysis. People who have ABI or SCI may require assistance to carry out activities of daily living. ABI and SCI
can also be linked to significant mental health issues, but not always. Early intervention and intensive care can make a difference in the long term outcomes.
Acquired
brain injury can result in problems with attention, planning and interacting with others. Spinal cord injury can lead to permanent paralysis. People who have ABI or SCI may require assistance to carry out activities of daily living. ABI and SCI
can also be linked to significant mental health issues, but not always. Early intervention and intensive care can make a difference in the long term outcomes.
Neurocritical care is the intensive care management of patients with life-threatening neurological and neurosurgical illnesses such as massive stroke, bleeding in or around the brain (subarachnoid hemorrhage, intracerebral hemorrhage, subdural hemorrhage, intraventricular hemorrhage), brain tumors, brain trauma, status epilepticus, nerve and muscle diseases (myasthenia gravis, Guillain-Barre Syndrome), spinal cord disorders and the cardiopulmonary complications of brain injury. Neurocritical care provides the interface between the brain and other organ systems in the setting of critical illness. Patients are taken care of within a single specialized unit. Neurocritical care units specialize in managing the unique needs of such critically ill patients.
There are numerous neurosurgical specialists working in these programs
Anschutz Neuro Critical Care Physicians
Robert Neumann, MD Director of Neuro Critical Care at CU Anschutz Campus |
Luis Cava Prado, MD |
David E Case, MD Neuro Critical Care Specialist at CU Anschutz |
VA & Pediatric Neuro Critical Care Physicians
Kathryn Beauchamp, MD Director of Neurotrauma at Denver Health Medical Center |
Kerry Brega, MD Director of Residency Program, CU Dept of Neurosurgery & Neurotrauma at the VA Medical Center, Anschutz Campus |
Brent O'Neill, MD, Director of Neurosurgery at Children’s Hospital of Colorado |
About Neurotrauma and the CU Department of Neurosurgery
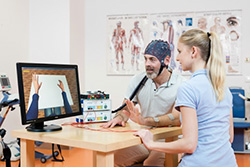 When
life is at stake, such as when there’s been a serious motor vehicle or motorcycle accident, or a serious brain injury resulting from an aneurysm or stroke, we know that life may never be the same. The Neurotrauma Center team at
CU’s Anschutz Medical Center (part of the region’s very few Level I trauma centers) offers the most comprehensive treatment available. With a wide range of subspecialists consulting and the regions expert neurosurgeons
available to provide immediate intervention, our team provides rapid assessment, diagnosis and treatment to lead to the best possible outcomes.
When
life is at stake, such as when there’s been a serious motor vehicle or motorcycle accident, or a serious brain injury resulting from an aneurysm or stroke, we know that life may never be the same. The Neurotrauma Center team at
CU’s Anschutz Medical Center (part of the region’s very few Level I trauma centers) offers the most comprehensive treatment available. With a wide range of subspecialists consulting and the regions expert neurosurgeons
available to provide immediate intervention, our team provides rapid assessment, diagnosis and treatment to lead to the best possible outcomes.
Denver Health Medical Center, formerly Denver General Hospital, has been an integral component of the University of Colorado since the founding of the medical school. DHMC is home to the Rocky Mountain Regional Trauma Center, the only Academic Level I Trauma Center in the region. DHMC is an internationally recognized trauma service, which provides multidisciplinary collaborative management of patients sustaining both blunt and penetrating injuries. The scope of neurosurgical services performed includes stabilization of spinal injuries involving all levels of the spinal column, and surgical management of traumatic brain injury.
The Rocky Mountain Region is fortunate to have The Children’s Hospital the only designated Level I Trauma Center in the region devoted and equipped to provide the highest standard of care for children. The five pediatric neurosurgeons affiliated with the Children’s Hospital of Denver are full-time faculty in the Department of Neurosurgery, having the full resources of a top academic department.
About Neuro Critical Care at CU/Anschutz
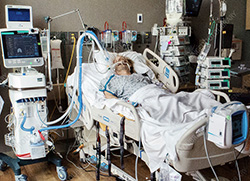 The
Neurosurgical Intensive Care Unit (Neuro ICU) at University of Colorado Hospital (UCH) is a regional referral center, and the only dedicated neurocritical care unit in the Rocky Mountain region. It is staffed twenty four hours per day with highly
specialized nurses and directed by three fellowship-trained neurocritical care specialists who are board certified by both United Council for Neurologic Subspecialties (UCNS) and Committee on Advanced Subspecialty Training (CAST). The 24-bed Neuro
ICU will soon be growing to 36 beds, and has over 1,300 admissions to our Neurosurgical ICU last year. We cater to those patients who need highly specialized, multi-disciplinary care.
The
Neurosurgical Intensive Care Unit (Neuro ICU) at University of Colorado Hospital (UCH) is a regional referral center, and the only dedicated neurocritical care unit in the Rocky Mountain region. It is staffed twenty four hours per day with highly
specialized nurses and directed by three fellowship-trained neurocritical care specialists who are board certified by both United Council for Neurologic Subspecialties (UCNS) and Committee on Advanced Subspecialty Training (CAST). The 24-bed Neuro
ICU will soon be growing to 36 beds, and has over 1,300 admissions to our Neurosurgical ICU last year. We cater to those patients who need highly specialized, multi-disciplinary care.
Under the leadership of Robert T. Neumann MD, PhD along with Luis Cava, MD., Josh Seinfeld, MD, Dave Case, MD, Chris Roark, MD and Wayne Gluf, MD, the practice has evolved to a leading subspecialty at UCH. As recipients of a Gold Beacon Award by the American Association of Critical-Care Nurses, the Neuro ICU team is recognized for excellence in sustained performance and patient outcomes.
The Neuro ICU team works seamlessly with Neurosurgical, Neurological, Interventional Radiology, General Surgery, Trauma, and Pulmonary and Internal Medicine specialties on a daily basis. The Neuro ICU provides all types of invasive and non-invasive cardiopulmonary, renal, and neurological life-support and monitoring. The technological advancements in the Neuro ICU provide the clinician, patient, and family with options and answers effecting quality of life.
The Neuro-Intensive Care Unit offers a Neurocritical Care Fellowship through both UCNS and CAST.
The Neuro ICU treatment team is dedicated to the advancement of neuro-critical clinical care. To this cause, the Neuro ICU attending physicians serve as Principal and Co-Investigators on multiple research projects, in both translational and clinical nervous system research. Included in these endeavors are: 1) evaluation of an in-series device that functions as a positive-end expiratory pressure relief valve, to augment cerebral circulation in ventilated patient with intracranial pressure monitoring; 2) evaluation of head positioning in acute stroke; 3) evaluation of the role of arginine deficiency in immune dysfunction following neurologic injury; 4) evaluation of non-invasive devices for early diagnosis of brain injury (including concussion), blood clot formation, and heparin-induced thrombocytopenia; 5) development of national standards for use of novel, FDA-approved neuro-critical care devices and therapeutics; and 6) advancing neural-grafting science.
 About
Stroke
About
Stroke
Stroke is one of the major diagnosis that we see and treat in neuro critical care, and on our Neuro ICU unit. Stroke is considered an acquired brain injury. For more information about our stroke program, stroke leadership, comprehensive stroke center, etc. please visit the CEREBROVASCULAR program under our “Programs of Excellence.” Patients may also want to visit “NEUROVASCULAR” under conditions we treat (Patient Resources).





