Contact UCHealth
Non-Hodgkin Lymphoma
Clinical Trials
Make a Gift
What Is Non-Hodgkin Lymphoma?
Non-Hodgkin lymphoma (NHL) is a cancer that starts in white blood cells called lymphocytes, which are part of the body’s immune system. According to the American Cancer Society, it is one of the most common cancers in the U.S., accounting for around 4% of all cancer cases. NHL can occur at any age, making it one of the most common cancers among youths and young adults, although the risk rises as we get older. It can either be aggressive or non-aggressive (indolent).
Non-Hodgkin lymphoma is one of two main types of lymphoma. It is more common than the other main type, known as Hodgkin lymphoma, and often is treated differently. Non-Hodgkin lymphoma accounts for about 90% of all lymphoma cases diagnosed.
NHL affects the lymph system (or lymphatic system), a network of organs, vessels, and tissues that serves as a key part of the body’s immune system and also helps filter waste products.
Lymphomas can start anywhere in the body where lymph tissue is found. That includes in hundreds of lymph nodes, which are tiny, bean-shaped glands in the lymph system that contain lymphocytes. Enlarged lymph nodes can be a sign of non-Hodgkin lymphoma, although the swelling is far more often caused by infections.
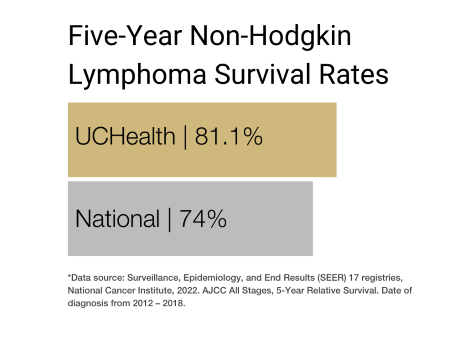
Non-Hodgkin Lymphoma Prognosis and Survival Rates
The American Cancer Society estimates that about 80,550 people will be diagnosed with non-Hodgkin lymphoma in 2023, and about one-fourth of those people will die from this cancer. Depending on various risk factors, a typical man has about a 1-in-43 chance of developing NHL in his lifetime; for women the rate is about 1 in 53.
Treatment varies depending on the type, stage (extent) and aggressiveness of the lymphoma. Treatment options might include chemotherapy, radiation therapy, immunotherapy, targeted drug therapy, and other options.
Why Come to CU Anschutz Cancer Center for Non-Hodgkin Lymphoma
As the only National Cancer Institute-designated Comprehensive Cancer Center in Colorado and one of only four in the Rocky Mountain region, the University of Colorado Anschutz Cancer Center has doctors who provide cutting-edge, patient-centered non-Hodgkin lymphoma care, and researchers focused on diagnostic and treatment innovations.
There are numerous lymphoma clinical trials being conducted by CU Anschutz Cancer Center members at any time. These trials offer patients alternatives to traditional lymphoma treatment and can result in remission or increased life spans.
→ Learn more about the lymphoma program at CU Anschutz Cancer Center
Types of Non-Hodgkin Lymphoma
Non-Hodgkin lymphoma (NHL) is largely categorized into two types, named for the type of white blood cell in which the cancer forms: B-cell lymphoma and T-cell lymphoma.
B-cell lymphoma
Around 85% of the NHL diagnosed in the United States are B-cell lymphomas — lymphomas that affect B lymphocytes, a type of lymphocyte that produces proteins called antibodies to attack diseases. The most common types of B-cell lymphomas include:
Diffuse large B-cell lymphoma, the most common type of NHL. It accounts for around one out of every three lymphomas. It earned this name because the lymphoma cells appear relatively large under a microscope.
Follicular lymphoma, which typically is a slow-growing (indolent) lymphoma, though some follicular lymphomas can grow quickly. Follicular lymphoma tends to occur in multiple lymph node sites in the body, as well as the bone marrow.
Chronic lymphocytic leukemia (CLL) and small lymphocytic lymphoma (SLL), which are closely related diseases that involve the same type of small lymphocyte. The biggest difference between the two has to do with where the cancer cells are found—in CLL, most are in the blood and bone marrow; and in SLL, cancer cells are found primarily in the spleen and lymph nodes.
Mantle cell lymphoma, a form of NHL that tends to be widespread in the bone marrow, lymph nodes, and often the spleen. Mantle cell lymphoma is more common in men than in women, and it most often occurs in people 60 and older.
Marginal zone lymphomas, which account for around 5% to 10% of all lymphomas. This form of NHL tends to be slow-growing (indolent). The three primary types of marginal zone lymphomas are:
- Extranodal marginal zone B-cell lymphoma, also known as mucosa-associated lymphoid tissue (MALT) lymphoma: The most common type of marginal zone lymphoma, this cancer starts in locations other than the lymph nodes, including the stomach, lung, skin, salivary glands, thyroid, or tissues around the eye.
- Nodal marginal zone B-cell lymphoma: This rare disease tends to start and stay in the lymph nodes, although cancer cells are sometimes found in the bone marrow.
- Splenic marginal zone B-cell lymphoma: This rare lymphoma is most often found in the spleen, blood, and bone marrow.
Burkitt lymphoma, a fast-growing form of NHL named for the doctor who first described the disease in children and young adults in Africa. Different varieties of Burkitt lymphoma are seen in different parts of the world:
- The endemic, or African variety of Burkitt lymphoma typically begins as a tumor of the jaw or other facial bones. Most cases of endemic Burkitt lymphoma are linked to infection with the Epstein-Barr virus. This disease is rare in the United States.
- Nonendemic, or sporadic Burkitt lymphoma is the variety seen more often in the U.S. The lymphoma most often begins in the abdomen, where it forms a large tumor. Nonendemic Burkitt lymphoma also can begin in the testicles, ovaries, or other organs and can spread to the brain and spinal fluid.
- Immunodeficiency-associated Burkitt lymphoma is associated with immune system problems such as HIV or AIDS or people who have had an organ transplant.
Lymphoplasmacytic lymphoma, a slow-growing form of NHL that accounts for just 1% to 2% of lymphomas. It is characterized by small lymphoma cells that are found primarily in the lymph nodes, spleen, and bone marrow.
Primary central nervous system lymphoma, which primarily involves the brain or spinal cord, though it is sometimes seen in tissues around the spinal cord.
Primary intraocular lymphoma, or lymphoma of the eye, a rare lymphoma that begins in the eyeball. It is often seen along with primary central nervous system lymphoma. It is the second most common eye cancer in adults, after ocular melanoma.
T-cell lymphoma
T-cell lymphomas make up less than 15% of non-Hodgkin lymphomas in the U.S. The most common T-cell lymphomas are:
Peripheral T-cell lymphomas, rare lymphomas that develop from more mature T cells.
Angioimmunoblastic T-cell lymphoma, which involves the lymph nodes and bone marrow, as well as the spleen or liver.
Extranodal natural killer/T-cell lymphoma, nasal type, a rare lymphoma that typically affects the upper airway passages, such as the nose and upper throat. It also can affect the skin, digestive tract, and other organs.
Enteropathy-associated intestinal T-cell lymphoma (EATL), a lymphoma that occurs in the lining of the intestine — most often the small intestine, but sometimes the colon.
Anaplastic large cell lymphoma (ALCL), which is more common in young people, including children, but it can also affect older adults. ALCL can affect the skin, lymph nodes, and other organs.
Adult T-cell leukemia/lymphoma, caused by infection with the HTLV-1 virus. It is more common in Japan, Africa, and the Caribbean. It affects the bone marrow, lymph nodes, liver, spleen, skin, and other organs.
Symptoms of Non-Hodgkin Lymphoma
Non-Hodgkin lymphoma doesn’t always cause symptoms in its early stages, and many of the symptoms it can cause are more likely to be signs of other conditions, such as infections. But if you have any of these common signs and symptoms, have them checked by a doctor:
- Swollen lymph nodes that might be felt as bumps or lumps under the skin, most often on the side of the neck, in an armpit, or in the groin.
- Chills.
- Unexpected weight loss.
- Unexpected fatigue.
- Swollen or painful abdomen.
- Feeling full after only a small amount of food.
- Loss of appetite.
- Chest pain or pressure.
- Shortness of breath or cough.
- Severe or frequent infections.
- Easy bruising or bleeding.
- A fever that comes and goes over several days or weeks, without an infection.
- Trouble thinking or speaking or personality changes (sometimes associated with lymphomas of the brain and spinal cord).
Diagnosing Non-Hodgkin Lymphoma
If you have any of the possible signs and symptoms listed under Risk Factors & Symptoms, particularly any lumps under the skin that haven’t gone away, have them examined by a doctor. Also, tell your doctor about any possible risk factors.
In an initial physical examination, the doctor will look for signs of enlarged lymph nodes. If any are found, the doctor will also look for signs of infection near the swollen nodes, since infection is the most common cause of enlarged lymph nodes. Because of this, the doctor may first prescribe antibiotics and wait a few weeks to see if the lymph nodes shrink before taking further steps. The doctor may also order blood tests to detect any infection or other problems.
Based on a patient’s symptoms and after the initial physical examination, a doctor may do a biopsy or other tests to determine whether the patient has non-Hodgkin lymphoma. Though testing procedures can vary, common screenings for lymphoma include:
Biopsy: A biopsy can confirm whether a person has NHL. During a biopsy, depending on the situation, a doctor may extract a piece of an enlarged lymph node (an incisional biopsy) or an entire lymph node (an excisional biopsy). These are sent to a laboratory for analysis by a pathologist to determine whether the cells in the sample are cancerous. These are the types of biopsy most commonly used if lymphoma is suspected in order to obtain enough of a tissue sample to diagnose the exact type of NHL.
If the node to be removed is just under the skin, a biopsy may be performed with only local anesthesia to numb the patient. But if the node is deep inside the chest or abdomen, it may be necessary to sedate the patient or administer general anesthesia.
There are other types of biopsy that a doctor might perform, such as a needle biopsy to help rule out infection as the cause of swollen lymph nodes, or other biopsies after NHL is diagnosed to determine its stage (extent) in the body.
Computed tomography (CT) scan: A CT scan is an imaging test that uses X-rays to take detailed images of the body and can help determine if any lymph nodes or organs are enlarged.
Positron emission tomography (PET) scan: Also a type of imaging test. A slightly radioactive form of sugar is injected into the blood, where it is taken in by cells in the body. Since cancer cells grow faster than normal cells, they take in larger amounts of the sugar. Doctors use PET scans to look for possible areas of cancer spread, and to determine if suspicious areas seen in other imaging tests are cancer or not. PET is considered the diagnostic imaging of choice for patients with aggressive lymphomas and some indolent lymphomas.
Ultrasound: This imaging test uses sound waves to create pictures of internal organs or masses. Ultrasound can be used to view lymph nodes near the surface of the body or to look inside the abdomen for enlarged lymph nodes or organs.
Stages of Non-Hodgkin Lymphoma
After diagnosing the presence of non-Hodgkin lymphoma, the doctor will identify the stage (or extent) of the cancer. The stage is determined by several factors, including where exactly the cancer formed and whether and how much it has spread. That information can aid in decisions on the best way to treat NHL.
Many of the tests used to diagnose NHL as described above also play a role in determining the cancer’s stage. Of these, generally the most important for staging purposes are imaging tests such as PET and CT scans.
The cancer’s stage is categorized under a system called the Lugano classification, based on an older system called the Ann Arbor classification. It has four stages, labeled by Roman numerals I through IV. Under stages I and II, if the lymphoma affects an organ outside the lymph system, it also is assigned the letter “E” for extranodal organ. Stage I and Stage II lymphomas generally are called “limited.” Stage III and Stage IV lymphomas usually are called “advanced.”
The stage can be important in determining treatment options for some types of NHL and less important for others.
Stage I: NHL is found only in one lymph node area or lymphoid organ such as the tonsils.
Stage IE: The cancer is found only in one part of one organ outside the lymph system.
Stage II: NHL is in two or more lymph node areas on the same side of (above or below) the diaphragm (the muscle band that separates the chest and abdomen). If a Stage II lymphoma involves large tumors in the chest, it often is described as “bulky,” and treatment decisions may be different than for “non-bulky” Stage II cancers.
Stage IIE: The cancer is in two or more lymph node areas and in one area of a nearby organ.
Stage III: NHL is in lymph node areas on both sides of the diaphragm, or the cancer is in lymph nodes above the diaphragm as well as in the spleen.
Stage IV: NHL has spread widely into at least one organ outside of the lymph system, such as the liver, bone marrow, or lungs.
Treatments for Non-Hodgkin Lymphoma
The treatment for non-Hodgkin lymphoma is customized to each patient and depends on the type of NHL, the stage at which the patient is diagnosed, and the patient’s general health. NHL care teams may include multiple health care specialists, including primary care providers, medical oncologists, hematologists, and radiation oncologists, as well as nurse practitioners, physician assistants, nurses, psychologists, social workers, and rehabilitation specialists. CU Anschutz Cancer Center doctors offer specialized care for patients with NHL.
Treatments for lymphoma include chemotherapy, radiation therapy, immunotherapy, and targeted drug therapy. Patients may receive one or more of these treatments in combination. Some patients may also be eligible to participate in clinical trials — doctor-led research studies of new or experimental procedures or treatments.
Chemotherapy for Non-Hodgkin Lymphoma
Chemotherapy is the main form of treatment for most NHL patients. It uses drugs to kill rapidly growing cancer cells. Drugs are either injected into a vein or taken orally. The drugs enter the bloodstream and are carried throughout the body, making it a particularly useful treatment for NHL.
Depending on the type and stage of lymphoma, chemotherapy (also called chemo) may be combined with immunotherapy or radiation therapy. Those factors also help to determine what drugs are used, what doses are administered, and how long the treatment continues.
Chemo is administered in cycles, with a period of treatment followed by a period of rest to allow time for the body to recover. Each cycle usually lasts for several weeks. Most chemo treatments are administered on an outpatient basis, but some involve a hospital stay.
Possible side effects of chemo, depending on drug type, dosage, and length of treatment, include:
- Hair loss.
- Mouth sores.
- Loss of appetite.
- Nausea and vomiting.
- Diarrhea or constipation.
- Increased chance of infection.
- Bleeding or bruising after minor cuts or injuries.
- Fatigue and shortness of breath.
Any such side effects usually go away after chemo treatment is concluded.
Radiation Therapy for Non-Hodgkin Lymphoma
Radiation may be an option as a main treatment for some types of NHL at an early stage (Stage I or II) that respond well to radiation. For more advanced or aggressive lymphomas, radiation might be used along with chemotherapy.
Radiation therapy usually involves a carefully focused beam of radiation to kill cancer cells. A doctor who specializes in radiation therapy to treat cancer is a radiation oncologist.
Radiation treatments often are administered over a period of several days to several weeks. The procedure, similar to getting an X-ray, is generally painless. Side effects can include redness or blistering of the skin, tiredness, nausea, or diarrhea.
Immunotherapy for Non-Hodgkin Lymphoma
Sometimes the body’s immune system does not attack cancer because cancer cells produce proteins that help them hide from immune system cells. Immunotherapy is intended to boost the patient’s immune system to help it attack and destroy cancer cells.
Several monoclonal antibodies are used to treat NHL. These are human-made versions of the proteins normally produced by the body’s immune system to fight disease. Monoclonal antibodies generally are designed to attack a specific target on the surface of lymphocytes, the immune-system cells where lymphomas start. Many of the monoclonal antibodies used against NHL target the CD20 antigen, a protein on the surface of some lymphocytes. They include:
- Rituximab (Rituxan).
- Obinutuzumab (Gazyva).
- Ofatumumab (Arzerra).
- Ibritumomab tiuxetan (Zevalin).
These drugs usually are administered into a vein over several hours. Most side effects are mild, including itching, chills, fever, nausea, rashes, fatigue, and headaches. Drugs administered before each infusion help ward off more serious side effects.
Another immunotherapy approach to treating NHL involves bispecific antibodies, a newer type of human-engineered antibody designed to attack two different targets. For example, T-cell engaging bispecific antibodies attach themselves to a protein on T cells, a type of immune cell, and also attach to a target on lymphoma cells. This helps the immune system attack lymphoma cells. There are many other types of engineered antibodies that can be used in treating NHL.
Another type of weapon against lymphoma cancer is the use of immune checkpoint inhibitors such as pembrolizumab (Keytruda) — drugs that help restore the immune system’s natural defenses against cancer cells. They block substances known as “checkpoints” on immune system cells that normally keep the cells from attacking healthy cells in the body, but which cancer cells sometimes use to avoid being attacked by the immune system.
Chimeric antigen receptor (CAR) T-cell therapy is a treatment in which immune cells called T cells are removed from the patient’s blood and altered in the lab to place receptors called chimeric antigen receptors, or CARs, on their surface. These receptors attach to proteins on the surface of lymphoma cells. The T cells are multiplied in the lab and put back into the patient’s blood, where they seek out and destroy NHL cells.
Targeted Drug Therapy for Non-Hodgkin Lymphoma
Targeted therapy focuses on the specific genes, proteins, or tissue environments that contribute to non-Hodgkin lymphoma, limiting damage to non-cancerous cells and tissues.
Here are some of the most common targeted drug therapies for NHL:
Proteasome inhibitors work by preventing enzyme complexes called proteasomes from breaking down proteins that help keep cell division under control. They are typically used to treat multiple myeloma but can be useful in treating some forms of NHL as well.
Histone deacetylase (HDAC) inhibitors affect which genes are active in a cancer cell by interacting with proteins in chromosomes called histones.
BTK inhibitors: Bruton’s tyrosine kinase is a protein that helps some lymphoma cells grow and survive. Targeting this protein and inhibiting its activity is useful in treating some types of NHL.
PI3K inhibitors work by slowing the processes of phosphatidylinositol 3-kinases (PI3Ks), a family of proteins that help regulate cell growth.
EZH2 inhibitors target EZH2, a protein called a methyltransferase that helps some cancer cells grow.
Nuclear export inhibitors block a protein that helps cells survive by carrying other proteins from the nucleus of a cell to other parts of the cell. When this process is blocked, it causes the cell to die.
Other Treatments for Non-Hodgkin Lymphoma
Surgery may be used to extract a biopsy sample to classify a lymphoma, but it’s rarely used as a treatment for NHL, except in some cases where the cancer has started in the spleen, thyroid, or stomach, and has not spread beyond these organs.
Small numbers of NHL patients are treated with higher-than-usual doses of chemotherapy coupled with a stem cell transplant (also known as a bone marrow transplant). Normally, doses of chemo drugs are limited because of their possible side effects, including damage to the bone marrow, where new blood cells are produced. But a stem cell transplant can make higher chemo doses possible because the patient receives blood-forming stem cells to restore the bone marrow afterwards.
Latest in Lymphoma from the Cancer Center
Information reviewed by Manali Kamdar, MD, in July 2025.