 Inworks lab’s 3D models of hearts to improve patient care while making it easier to explain procedures to patients and their families.
Inworks lab’s 3D models of hearts to improve patient care while making it easier to explain procedures to patients and their families.
Model Hearts and Virtual Reality
Inworks lab brings advanced technology to patient bedside
By Joseph Carrillo

Lorna Brown, MD
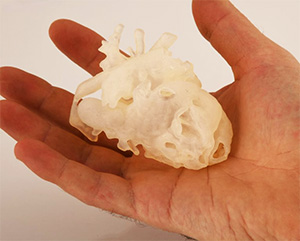
(May 2020) Lorna Browne, MD, holds an intricately detailed 3D printed model of a child’s heart.
With each chamber and valve rendered in a rainbow of colors and translucency, it would be easy to mistake the anatomical model as a work of art. Just a few years ago, this type of model was unimaginable.
Now, such models are used by CU School of Medicine faculty at Children’s Hospital Colorado to rethink approaches to pre-operative planning and to improve the quality of bedside care for patients and their families.
Such models are the result of decades of advancement in radiology scanning and more recent leaps in 3D printing. “It’s a really exciting field,” said Browne, who is professor of radiology at CU School of Medicine and a pediatric radiologist at Children’s Hospital Colorado on the Anschutz Medical Campus. “There are so many technical advancements to be involved in.”
At the cutting edge of this printing is Nick Jacobson and the Inworks prototyping lab, also located on the Anschutz Medical Campus in the Strauss Health Sciences Library. Inworks is an innovation initiative of the University of Colorado Denver | Anschutz Medical Campus, providing a home for creators, thinkers, designers, and makers. Drawing on experts from many disciplines, Inworks offers learning and teaching through making things that matter.

James Joseph Thomas, MD
Browne offers another model, this one of an 18-month-year old’s crisscross heart, a rare cardiac malformation characterized by crossing of the inflow streams of the two ventricles due to an apparent twisting of the heart about its long axis.
“As you can imagine, just seeing this in two dimensions, it’s very hard to understand and figure out how to rearrange the blood vessels,” she said, explaining the advantages that the physical model holds over a traditional computer model.
“You can move structures in a way you can’t on just a screen, you can even practice the surgery by doing incisions,” Browne said. With this tool in hand, medical professionals such as Browne are able to plan surgeries in a more tangible way than ever before and have a better understanding of how the patient may respond to the procedure.
Being able to manipulate a 1:1 replica of a patient’s heart, before making a single incision, is an invaluable tool for any surgeon and an obvious advantage of this type of 3D printing.
What may not be so obvious is the advantage the tangible model has on doctor-patient relations.
“You can also show this to the patient’s family, and the surgeon can say, ‘This is what it looks like and this is what I’m going to do,’ and that’s a huge thing. It’s an incredibly stressful situation having your child operated on.”
Jenny Zablah, MD, an assistant professor of pediatric cardiology at CU School of Medicine, agreed that the benefits of 3D printing are expansive. “It’s complementing what we already know from the angiograms [and] from, the patient’s perspective, it helps them understand their anatomy.”
Zablah has broken new ground by taking the images produced by angiogram and printing 3D models in her office. These models serve to assist the medical team planning the operation and the families of patients, who might be feeling left in the dark when it comes to the specifics of the procedure.
When treating patients, especially children, trust in the doctor performing these medical procedures can drastically alter the experience for the medical professional and patient. 3D printed models can encourage and facilitate more effective dialogue between families and doctors, allowing all parties involved to better understand what procedures will be performed and what the outcomes might be.
“I process the images and print them right in my office. The printing usually takes about 24 hours,” Zablah explained, “The patients are happy with seeing these models before the operation. It provides a nice memory or memento during a difficult time.”
In addition to putting minds at ease, these models also reduce the time patients are exposed to radiation while undergoing imaging. By having a physical model that can be referenced repeatedly throughout pre-operation planning, physicians are able to reduce the number of times an individual may need to undergo imaging procedures and in turn reduce the risk of repeated radiation exposure. In tandem with other technologies such as virtual reality, patients are receiving care that reduces the risk of complications.
 As James Joseph Thomas, MD, an assistant professor of anesthesiology at CU School of Medicine and colleague of Browne and Zablah said, “Some of these cath lab procedures
we could potentially do with no sedation or without general anesthesia, or with minimal sedation, because of the power of the distraction of virtual reality systems.”
As James Joseph Thomas, MD, an assistant professor of anesthesiology at CU School of Medicine and colleague of Browne and Zablah said, “Some of these cath lab procedures
we could potentially do with no sedation or without general anesthesia, or with minimal sedation, because of the power of the distraction of virtual reality systems.”
Anesthesia can change the physiology of the patient, which is then treated with more drugs, so having a tool like a VR system can lead to a reduction in the number of drugs a patient needs to take. Reducing the amount of drugs administered to a patient is a particularly optimal goal when that patient is a child and may be receiving multiple tests or procedures in a single day.
Children’s Hospital Colorado has already seen wide success with virtual reality distraction, reducing the need for sedation and general anesthesia in some cases. The value of this is twofold as a calm and cooperative patient puts less pressure on medical staff, ensuring they are able to complete their tasks in the most effective way possible.
“A big part of introducing these kinds of technologies into the health care realm is creating experiences for doctors and patients [and] using this technology as a tool to improve our bedside manner,” Thomas said.
For Thomas, the advent of 3D printing is only one tool in closing the gap between doctor and patient understanding. Browne, Zablah, and Thomas hope to use advances in technology in tandem with 3D printed models to ease the minds of patients and family alike.
“We’ve been talking about some ideas of creating these 3D models in virtual reality, so it’s just a file we can share with the family and they can take it home and potentially look at it in a 3D headset and share it with their family,” said Thomas, “We’re using these technologies as a tool to help capture [the patient’s] attention and pull it away from this thing that may be causing them anxiety and stress.”
Whether it is VR used to create calming distractions of the virtual or 3D printing to provide a tangible model that makes it easier to understand a procedure, the progression of technology is offering an array of solutions to medical obstacles.
“When you have a sick child, it’s one of the worst things you can go through,” said Thomas. “If you can, in any way, make that entire situation easier for the patient and their families, the impact that has on their lives is enormous. That’s why we went into pediatrics: to try to make those difficult times better and easier.”
Feature Stories
- Building Professional Resilience Through Creative Arts
- Model Hearts and Virtual Reality
- Improving Care for Colorado; CU School of Medicine expands access to care statewide
- New Clinic is ‘Bigger than What’s in These Four Walls’
- Innovative Palliative Care Fellowship Program
- Leadership, Curiosity, Commitment; School of Medicine updates curriculum for medical students
- Student Voice: The Gift of Gratitude
- Faculty Matters: What Every Doctor Should Know About the Holocaust
Profiles
- Searching For Cures to Lung Diseases
- Osseointegration surgery offers hope for better, faster, stronger life
- Building a Team, Not Just a Building; Hospital leader receives life-saving care after stroke at work