Making Connections
Telehealth improves access for rural patients
By Megan Lane
 (December 2017) As Bettina Cuneo, MD, peered intently at an
(December 2017) As Bettina Cuneo, MD, peered intently at an
But this was no ordinary doctor’s appointment.
The previous week, during her 20-week ultrasound, the woman had been told that her baby might have a heart defect, so she was referred for further evaluation to Cuneo, a renowned fetal cardiologist at the Colorado Fetal Care Center at Children’s Hospital Colorado and professor of pediatrics at the CU School of Medicine.
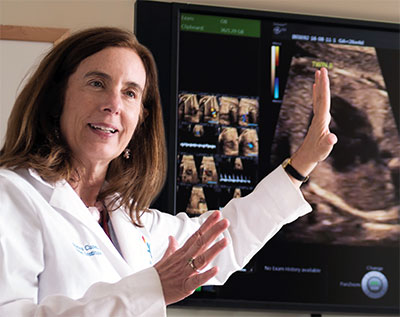
As Cuneo viewed real-time ultrasound images in her clinic in Aurora, her patient was sitting with an ultrasound technician in Grand Junction, 250 miles away. Using video conferencing technologies, Cuneo could see live imaging of the baby.
This “virtual clinic” for fetal heart anomalies has saved expectant mothers hundreds of hours of driving time and countless moments of worry.
After discussing the patient’s history and concerns through the video conference line, Cuneo directed the ultrasound technician to zoom in on a specific area of the baby’s heart. Cuneo adjusted the volume on her monitor, allowing her to hear the baby’s heartbeat as clearly as if she were sitting right next to the patient. She closed her eyes, listened closely, and then looked directly into the video camera.
“Your baby is going to be fine,” Cuneo said.
Through the image on her video screen, Cuneo could see tears of relief in the mother’s eyes.
Improving Access
Using digital tools and programs, caregivers can provide long-distance clinical care and health education. With telecommunications technologies, they reach patients in homes, schools, workplaces
“I think of telehealth as healing from a distance,” said Cuneo. “I love that I can help to reassure someone without making them drive all the way across the Continental Divide.”
The growth in telehealth comes when millions of Americans face challenges accessing health care. Many rural areas lack child and maternal health providers even as studies show that kids treated by caregivers with pediatric training and experience have better health care outcomes. Moreover, research indicates that children and pregnant mothers receiving treatment closer to home fare better than those traveling long distances.
In response, Children’s Colorado has launched new telehealth programs: a virtual consultation with a pediatric specialist, a smartphone app that encourages healthy behaviors, and technology that allows a doctor to track a child’s vital signs from hundreds of miles away.
“Improving access is one of the greatest benefits of telemedicine,” said Fred Thomas,
Philanthropy makes it possible
The upfront investment in new virtual health programs and can be significant, and traditional reimbursement and funding models often don’t support the
“The proof of concept has to happen first, and that’s where philanthropy is absolutely critical,” said Thomas.
Philanthropy has played a significant role in establishing and maintaining these programs at Children’s Colorado. One example is a partnership with a pediatric practice in Durango, which gives virtual access to pediatric specialists at Children’s Colorado for area children with complex care needs. With digital otoscopes and stethoscopes, Children’s Colorado specialists conduct full exams on patients hundreds of miles away.
“It can be extraordinarily burdensome for these children to access the pediatric specialty care they require,” said Thomas, noting that rural families often spend days commuting to and from Children’s Colorado, missing work and school and incurring costly travel expenses. “With telehealth, patients can go right down the road to see their sub-specialist instead of coming to Denver.”
Children’s Colorado continues to develop partnerships with rural providers across the region, allowing them to more easily consult with our expert sub-specialists on complex pediatric health issues.
“We’re the only organization in the country that’s doing the array of what we’re doing,” said Thomas. “Telehealth is all about innovation and stretching the limits of what’s possible. I think this is one of the most life-altering things we do at Children’s Colorado.”
This article was originally published in July by the Children’s Hospital Colorado Foundation.