Tell Me More
Gold Humanism program encourages compassionate care
By Debra Melani
(May 2018) In the end, his patient died.
But as Ajay Major, MD, MBA, then an intern, flipped through the old veteran’s medical record, he found comfort in the memories the notes inspired.
Major, now a second-year internal-medicine resident on the University of Colorado Anschutz Medical Campus, calls up those memories of the witty old man with terminal cancer who always asked for bourbon (and his devoted wife who always rolled her eyes in response), as a reminder of the importance of compassion in health care.
“Medicine is hard,” Major said. “We see a lot of patients with a lot of difficult medical issues, and I think burnout stems not just from feeling overworked, but also from feeling that we’re not truly caring for our patients on a human level.”
Major, co-president of the CU Anschutz School of Medicine Resident Chapter of the Gold Humanism Honor Society, spread his message during the society’s annual Solidarity Week in February by encouraging his colleagues to take part in the week’s centerpiece program, Tell Me More.
Changing the conversation
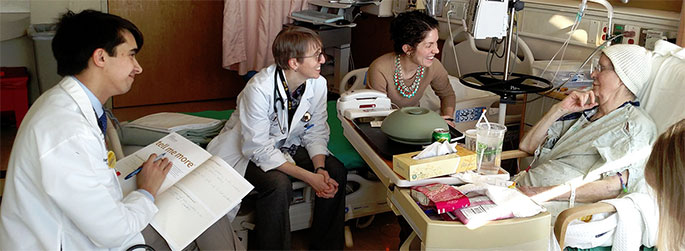
Armed with a questionnaire and a smile, second-year internal-medicine resident Megan Griff, MD, entered her patient’s room, finding Betty Redwine, 77, wrapped in a light blanket and relaxing in a chair. “Is it OK to talk and find out about your life?” Griff asked, after explaining the program and introducing Major and attending physician, Jeannette Guerrasio, MD.
“OK,” Betty Redwine said, returning her doctor’s smile. “But it’s nothing exciting,” she said, grinning up from beneath a black-suede, shower-like cap that she informed her guests was taming her unruly hair.
Prompted by four Tell Me More questions, Redwine soon was sharing pieces of her past. Discussions of capillaries and high blood pressure gave way to remembrances of children’s feats and life’s treasures, sounding more like tea-time chatter than bedside diagnoses. When Redwine let a little secret slip, the room filled with utterances of disbelief.
“What?” Guerrasio
Staying centered on the cause
While it might seem small, a dose of compassion can result in an array of benefits, Major said.
“It allows the patient to feel that the care team really cares about them, but it also brings some catharsis for providers,” Major said. “Just finding out a little bit more about our patients’ lives outside of the hospital can help re-center us in the work that we are doing as physicians and, I believe, help prevent burnout.”
On the patient side, studies show compassionate healthcare results in higher patient satisfaction, a higher pain threshold, reduced anxiety and better outcomes, according to the Arnold P. Gold Foundation, which is named after a renowned pediatric neurologist who became an international leader and
“People develop diseases for lots of reasons, and everyone’s lives really affect the way they respond to health problems,” said David Schwartz, MD, chair of the Department of Medicine. It makes sense that patient-provider relationships based on trust result in better care, he said. “We need to know how their lives might be contributing to the development of disease, and how their lives might contribute to our ability to effectively treat their disease,” he said.
Remembering: ‘I’m a person’
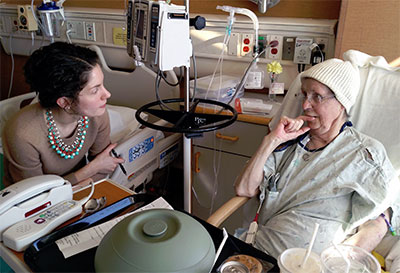 Looking up from her bed as the Tell Me More trio walked into her room, Frances Cory, 79, had them laughing before even agreeing to chat. “You want to talk beyond my medical condition? You mean you don’t care about my medical condition anymore?” said the mother and grandmother, who later responded to a question about her biggest strength: “My sense of humor.”
Looking up from her bed as the Tell Me More trio walked into her room, Frances Cory, 79, had them laughing before even agreeing to chat. “You want to talk beyond my medical condition? You mean you don’t care about my medical condition anymore?” said the mother and grandmother, who later responded to a question about her biggest strength: “My sense of humor.”
Cory, who shared with her visitors that she had served more than 5,000 volunteer hospital hours during her lifetime, said she thought the program was important. “It’s nice to know that you take the time to talk to your patients. I’m a person.”
The Tell Me More program offers a valuable reminder for medical providers that their patients are people, and not just medical mysteries to solve, Guerrasio said. “I actually, as a doctor, find these conversations really helpful. And it’s what makes me come to work every day.”
Notes about the patient-doctor chat are jotted down on the Tell Me More questionnaire, which is then displayed on the wall so that everyone involved in that patient’s stay, from therapists and nurses to doctors and janitors, can use it as conversation fodder, Major said.
Seeing nothing as too small
By getting to know his end-stage cancer patient and his wife as an intern, Major learned not just about his patient’s bourbon routine, but that he was a strong war veteran who had “always been a fighter.” That helped
When his patient was transferred to hospice, Major told the palliative caregivers about his patient’s taste for bourbon. Looking through his patient’s medical record after learning of his death, Major was jolted by one caretaker directive: Bourbon, one ounce at
“It seems like such a small detail,” said Major, who published an article in JAMA Oncology about the patient experience. “But when