Foothills Clerkship Phase
What is a Longitudinal Integrated Clerkship?
Per the International Consortium of Longitudinal Integrated Clerkships: A clinical curriculum in which students participate in comprehensive care of patients over time, engage in continuity relationships with preceptors and evaluators, and meet core clinical competencies across multiple disciplines simultaneously.
How is the LIC structured?
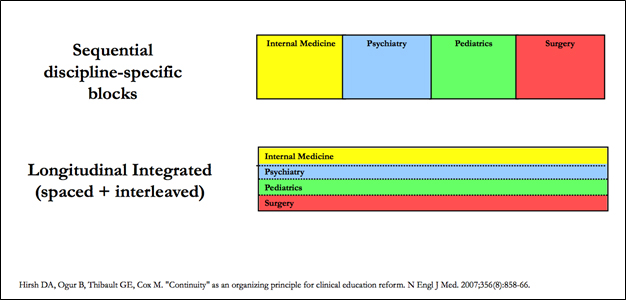
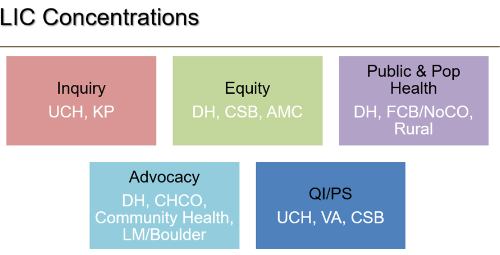
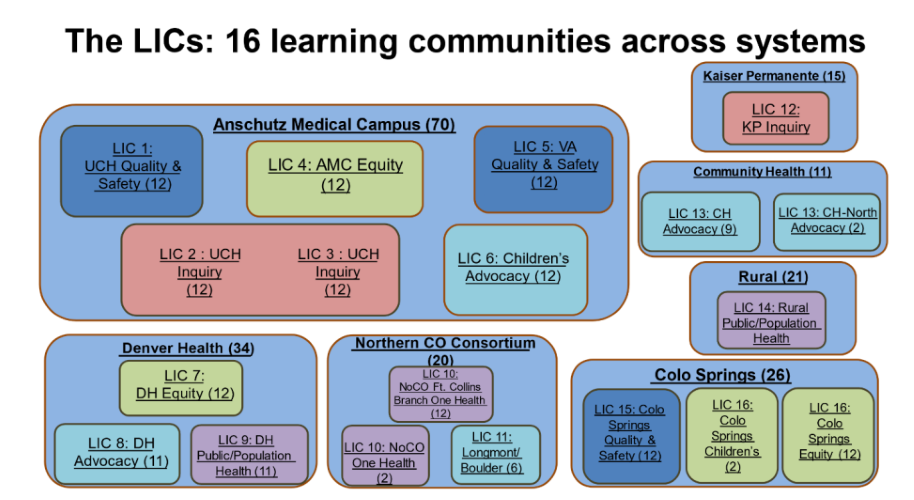
Students will spend their second year of medical school placed in an LIC in a single health care setting and system. An LIC creates a learning community of students and faculty and allows students to work with the same preceptor in each specialty all year providing longitudinal teaching, mentorship and assessment. Students develop a cohort of patients from all specialties that they follow through primary care, subspecialty clinics, inpatient, and emergency settings throughout their year in the program.
Students participate in shortened inpatient “immersions” in surgery, medicine, labor and delivery, gynecology, pediatrics, and psychiatry. The remainder of the year is dedicated to longitudinal, integrated clinical experiences working one-on-one with faculty preceptors in every specialty. Students are given ample unstructured time for independent learning, follow up with cohort patients, and professional development. Students participate in weekly small group didactic and workshop series focusing on core clinical topics and unique LIC curricular content.
 Foothills Goals
Foothills Goals
By immersing all medical students at the University of Colorado Anschutz School of Medicine in Longitudinal Integrated Clerkships (LICs), we aim to foster learning communities during the critical clerkship year that will create supportive learning environments with strong mentorship, individualized feedback, and provision of authentic and longitudinal roles in patient care. The LICs will support students’ personal and professional development through coaching and longitudinal preceptor relationships, positive role-modeling and engagement in an integrated case-based curriculum which threads critical concepts in basic medical science and health & society into a clinical care framework. Students will ask and answer complex patient care questions applying evidence-based medicine, incorporate principles of public health into the care of patients and communities, consider social determinants of health in individualizing care for patients, understand health care system science as it applies to the safe and effective care of patients, and develop as strongly committed patient advocates. Students will emerge from their Foothills training ready to embark on the individualized phase of the Trek curriculum as curious and independent learners with a robust foundation in clinical medicine.
Office of Curriculum Contact Information
|
|