Reclaim™ Deep Brain Stimulation (DBS) Therapy for Obsessive-Compulsive Disorder (OCD)
The University of Colorado Anschutz (with University of Colorado Hospital) is one of the few centers in the U.S. to offer Deep Brain Stimulation as an option for treatment-refractory obsessive-compulsive disorder. The CU Anschutz program offers a multi-disciplinary approach through collaboration with the Departments of Psychiatry, Neurology, and Neurosurgery.
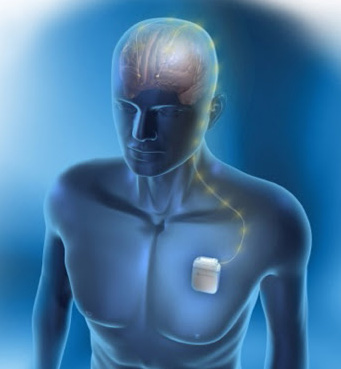
Deep Brain Stimulation involves a stereotactic neurosurgical procedure to place electrodes in both sides of the brain in structures known as the Anterior Limb of the Internal Capsule (AIC). The areas that are specifically targeted within the AIC are the Ventral Capsule/Ventral Striatum (VC/VS) and Nucleus Accumbens (NAc). The electrodes are connected to extension wires and pulse generators (similar to pacemakers) in the individual's chest wall. After surgery, the patient works with a psychiatrist with expertise in DBS programming to find the stimulation settings that provide optimal relief of symptoms with minimal side effects.
DBS of the Anterior Limb of the Internal Capsule (AIC) is approved under the U.S. FDA Humanitarian Device Exemption (HDE) for severe to extreme treatment-resistant OCD:
An HDE is a determination that a medical device is safe and has probable benefit. An HDE device is not considered investigational or experimental. HDE products are considered by the FDA to be commercially approved and are eligible for coverage and payment when an Institutional Review Board (IRB) approval exists at the facility performing the procedure.
If you are interested in DBS for severe, treatment-refractory OCD, please have your primary psychiatrist complete this form and fax to 303-724-8859. If you have questions, please call (303) 724-4716 and provide your phone number and email so you can be contacted by our DBS Coordinator.
An individual, 18 years-old or older may be a candidate for treatment with DBS if he or she meets the following criteria:
- Severe to extreme OCD (Yale-Brown Obsessive Compulsive Scale score of 28 or higher)
- Has participated in at least 20 sessions of exposure and response prevention therapy with an OCD specialist
- Has tried at least three serotonergic medications (such as SSRIs) at FDA-max dose or higher for at least 12 weeks each at max dose. One of these agents needs to be clomipramine with a therapeutic blood level for 12 weeks.
- Has taken a long-acting benzodiazepine in addition to a serotonergic medication for at least a month
- Has taken an antipsychotic (dopamine blocking medication) in addition to a serotonergic medication for at least a month
- Does not have any active substance use disorder
- Does not have a severe personality disorder
- Does not have a primary psychotic or bipolar disorder
- No imminent suicidality (no recent or current suicidal behaviors or plans)
If you are interested in DBS for severe, treatment-refractory OCD, please have your primary psychiatrist complete this form and fax to 303-724-8859.
Frequently Asked Questions
- What if I’m not working with a psychiatrist?
In order to be considered for DBS you need to establish care with a psychiatrist or other psychiatric prescriber who can manage your medications and can give us a medical and clinical overview of your psychiatric history. All referrals for DBS must come directly from a treating provider.
- What if I’ve had multiple psychiatrists/prescribers?
We only need your current prescriber to complete the referral form. If you’ve had multiple prescribers, please work with your current prescriber to collect and provide as much information on your medication and psychiatric history as possible.
- Does insurance cover DBS?
Under Mental Health Parity laws, DBS should be covered by insurance. However, coverage does vary based on insurance. We have had insurance companies be extremely cooperative and at other times not so much. Please contact your insurance company to request information about coverage for DBS for OCD. We are happy to help you with the authorization process, but please be aware that approval for DBS has sometimes taken more than a year and, other times, is not approved at all.
- Can I get surgery somewhere else and then programming with CU Anschutz?
No. We require all patients who receive programming with us to also complete their surgery at our hospital. This allows us to provide the most efficient and high-quality care for you. If you are already established with a center (including programming) then move to Colorado or a nearby state, we will consider taking over your follow-up DBS care.
- I meet all the criteria, except for medication requirements. Can exceptions be made?
No. Exceptions around medication criteria cannot be made. DBS is an invasive brain surgery. In order to qualify for DBS, you must have exhausted treatment options, including medication trials. If you have tried clomipramine and did not tolerate it well due to severe side effects (such as heart problems or seizures, not just anxiety/distress around taking it), this counts as a medication trial.
- If I have bipolar disorder and OCD, can I still receive DBS with CU Anschutz?
No. Bipolar disorder can be exacerbated by DBS.
- I have a co-occurring psychiatric diagnosis; can I still receive DBS with CU Anschutz?
Yes. However, any suicidality cannot be imminent and highly active. A substance use disorder must not be currently active. Psychosis and psychotic disorders cannot be the primary diagnosis and must be currently managed or at least being treated. A co-occurring eating disorder must be either in remission, actively being addressed and treated, or medically stabilized.
- Can the intake with the team be done virtually?
Our team typically finds it important for the first meeting to be in person. That way, they can get to know you and your support system effectively. If this is not possible, exceptions can be made on a case-by-case basis.
- How soon can I have surgery?
This depends on several factors. One factor is how quickly we receive your referral form and information to review. IF you are found to be a potentially appropriate candidate, there are also several meetings and tests that you will need to undergo over several months. Your case must then be reviewed by the ethics committee, and your insurance has to authorize the procedure.
- What is the time commitment for DBS?
Beyond the above and the surgery, DBS is a big commitment. At one point between your first two surgeries, you will be required to meet with our DBS coordinator to do psychological assessments for a 30-60 min appointment. Your first week of programming takes place about a month after your second surgery. This requires you to attend 3 in-person programming sessions that week. After that, you will attend programming once a week for about a month. The frequency of programming will decrease over time based on your response and the team’s clinical opinion.
OCD Ruled Moksha Patel’s Life Until a Rare Surgical Procedure Changed Everything
School of Medicine instructor Patel, with support from colleagues and other healthcare experts, sought deep brain stimulation to help escape the confines of OCD
OCD Patients with Comorbidities Respond Well to Deep Brain Stimulation
A critical study examines how patients with psychiatric comorbidities respond to Deep Brain Stimulation treatment for Obsessive Compulsive Disorder.
Contact Us
Department of Psychiatry OCD Program
University of Colorado Anschutz
1890 N Revere Ct
Anschutz Health Sciences Bldg, Suite 5040
Aurora, CO 80045
Phone: (303) 724-4716
For Outpatient call (303) 724-4716 or email [email protected]
Email for IOP questions and information: [email protected]
Rachel A. Davis, MD
Medical Director, OCD Program
Service Director, Psychiatric Neuromodulation
Emily Hemendinger, LCSW, MPH, CPH, ACS
Clinical Director, OCD Program
DBS Coordinator
Other Resources: ERP Course Website