Old News and Achievements Archive
Drs. Brian Montague and Michael Haden lead the I.D. Fellowship Training Program
 In July 2022 Dr. Brian Montague took on the I.D. Fellowship Program Director role alongside Dr. Michael Haden as Associate Program Director. Dr. Montague served as Associate Program Director for two years before stepping into the Program Director role and we thank Dr. Montague and Dr. Haden for their leadership. We extend gratitude to Drs. Katherine Frasca, Carlos Franco-Paredes, Dave Beckham, and Kristine Erlandson for their contributions in prior years. Many thanks also to Chelsee McFarland for her service as our Education Coordinator.
In July 2022 Dr. Brian Montague took on the I.D. Fellowship Program Director role alongside Dr. Michael Haden as Associate Program Director. Dr. Montague served as Associate Program Director for two years before stepping into the Program Director role and we thank Dr. Montague and Dr. Haden for their leadership. We extend gratitude to Drs. Katherine Frasca, Carlos Franco-Paredes, Dave Beckham, and Kristine Erlandson for their contributions in prior years. Many thanks also to Chelsee McFarland for her service as our Education Coordinator.
Dr. Mamuka Kvaratskhelia gave an oral presentation at the 2022 Cold Spring Harbor Retroviruses Meeting on May 25
 Mamuka presented quite novel findings on the intranuclear mechanism of action of the exceptionally potent, long-acting, new antiretroviral drug lenacapavir. His lab discovered that this HIV-1 capsid-binding drug acts mainly after viral nuclear entry, by hyper-stabilizing and functionally compromising the pliability of the capsid. Previously the mechanism was thought to be interfering with binding of cellular factors in the cytoplasm or nucleus.
Mamuka presented quite novel findings on the intranuclear mechanism of action of the exceptionally potent, long-acting, new antiretroviral drug lenacapavir. His lab discovered that this HIV-1 capsid-binding drug acts mainly after viral nuclear entry, by hyper-stabilizing and functionally compromising the pliability of the capsid. Previously the mechanism was thought to be interfering with binding of cellular factors in the cytoplasm or nucleus.
Dr. Katharine Frasca gave DOM Grand Rounds on May 25, 2022 on the topic of "Advances in HIV PrEP."
 Katharine reviewed the rationale and supporting data for the
effectiveness of this important preventive intervention, as well as
practical aspects of implementation and use. Health care disparities and
their relationships to care barriers and outcomes were also
illuminated. The PrEP Program newsletters are provided at a separate
link on this page.
Katharine reviewed the rationale and supporting data for the
effectiveness of this important preventive intervention, as well as
practical aspects of implementation and use. Health care disparities and
their relationships to care barriers and outcomes were also
illuminated. The PrEP Program newsletters are provided at a separate
link on this page.
Congratulations to Dr. Larissa Pisney for Receiving the 2022 Partners in Care Award
The award from the University of Colorado Hospital recognizes an employee for outstanding contributions as a productive member of the care team or for consistently offering amazing service to the medical staff through the course of their job duties.
Dr. Steven Johnson Recognized by Drs. Fauci and Collins for Contributions to NIH COVID-19 Treatment Guidelines
 Steven Johnson, MD, Professor of Medicine, was recognized last week by leaders of the National Institutes of Health
for his contributions to the NIH “Coronavirus Disease 2019 (COVID-19) Treatment Guidelines.” On December 8, NIH Director Francis S. Collins, MD, PhD, and Anthony S. Fauci, MD, director of the National Institute of Allergy and Infectious
Diseases, said that the guidelines are the gold standard that have accrued more than 27 million page views as of late November. They wrote: “Your expertise has been invaluable. Your devotion to the process, participating in virtual meetings
that typically occurred multiple times per week, and numerous hours spent in writing and editing content, are much appreciated.” They credited Steve and his fellow contributors’ efforts as resulting in guidelines that have “substantial
national and international impact.”
Steven Johnson, MD, Professor of Medicine, was recognized last week by leaders of the National Institutes of Health
for his contributions to the NIH “Coronavirus Disease 2019 (COVID-19) Treatment Guidelines.” On December 8, NIH Director Francis S. Collins, MD, PhD, and Anthony S. Fauci, MD, director of the National Institute of Allergy and Infectious
Diseases, said that the guidelines are the gold standard that have accrued more than 27 million page views as of late November. They wrote: “Your expertise has been invaluable. Your devotion to the process, participating in virtual meetings
that typically occurred multiple times per week, and numerous hours spent in writing and editing content, are much appreciated.” They credited Steve and his fellow contributors’ efforts as resulting in guidelines that have “substantial
national and international impact.”
Dr. Castillo-Mancilla to be Associate Medical Director of the Adult CTRC
 Dr.
Jose Castillo-Mancilla, MD has been appointed Associate Medical Director of the Clinical and Translational Research Centers of the CCTSI. He will oversee the adult CTRC at UCHealth under the leadership of Medical Director Dr. Tom Campbell. An Associate
Professor of Medicine. Dr. Castillo-Mancilla is an NIH-funded clinical researcher in antiretroviral adherence and clinical pharmacology, and a co-investigator in the AIDS Clinical Trials Group (ACTG). At the ACTG he co-chairs a large multicenter clinical
trial focused on novel therapeutic strategies for persons living with HIV who face barriers to adherence.
Dr.
Jose Castillo-Mancilla, MD has been appointed Associate Medical Director of the Clinical and Translational Research Centers of the CCTSI. He will oversee the adult CTRC at UCHealth under the leadership of Medical Director Dr. Tom Campbell. An Associate
Professor of Medicine. Dr. Castillo-Mancilla is an NIH-funded clinical researcher in antiretroviral adherence and clinical pharmacology, and a co-investigator in the AIDS Clinical Trials Group (ACTG). At the ACTG he co-chairs a large multicenter clinical
trial focused on novel therapeutic strategies for persons living with HIV who face barriers to adherence.
Dr. Mary Bessesen Awarded 2021 Golden Stethoscope Award
 Professor
Mary Bessesen has been awarded a 2021 Golden Stethescope award for her leadership during the COVID-19 pandemic at the Rocky Mountain Regional VA Medical Center. Her nominator, Medical student Lauren Heery, wrote: "As I begin the process of applying
to Internal Medicine residency this year, I hope that I can model my career after Dr. Bessesen's leadership. Her attentive and compassionate teaching, patient care, and leadership are all skills I hope to emulate in my training. The impact of
Dr. Bessesen's leadership and mentorship extends to so many students, colleagues, and patients, and this award is well-deserved!" More information on the Golden Stethescope Awards can be found here.
Professor
Mary Bessesen has been awarded a 2021 Golden Stethescope award for her leadership during the COVID-19 pandemic at the Rocky Mountain Regional VA Medical Center. Her nominator, Medical student Lauren Heery, wrote: "As I begin the process of applying
to Internal Medicine residency this year, I hope that I can model my career after Dr. Bessesen's leadership. Her attentive and compassionate teaching, patient care, and leadership are all skills I hope to emulate in my training. The impact of
Dr. Bessesen's leadership and mentorship extends to so many students, colleagues, and patients, and this award is well-deserved!" More information on the Golden Stethescope Awards can be found here.
Lorna Allen Wins Shark Tank
 Assistant
Professor of Medicine Lorna Allen, FNP, has won this year's Annual DOM Shark Tank Competition for her Quality Improvement project "VECTORS:
Vancomycin Errors Corrected Through Optimizing OPAT Med Reconciliation and AVS Standardization." Congratulations to her on this achievement. The Division also thanks her for all her superb, fastidious, and very hard work to make our outpatient
antimicrobial therapy (OPAT) program a success. The project has identified and proposes specific solutions for common, important issues related to delivery of the antibiotic vancomycin to outpatients. As this year's Shark Tank winner, she will
receive one year of quality coaching, project management, data collection and Epic analyst support, and stakeholder support. This project has great potential to optimize patient care and simplify logistics for our providers.
Assistant
Professor of Medicine Lorna Allen, FNP, has won this year's Annual DOM Shark Tank Competition for her Quality Improvement project "VECTORS:
Vancomycin Errors Corrected Through Optimizing OPAT Med Reconciliation and AVS Standardization." Congratulations to her on this achievement. The Division also thanks her for all her superb, fastidious, and very hard work to make our outpatient
antimicrobial therapy (OPAT) program a success. The project has identified and proposes specific solutions for common, important issues related to delivery of the antibiotic vancomycin to outpatients. As this year's Shark Tank winner, she will
receive one year of quality coaching, project management, data collection and Epic analyst support, and stakeholder support. This project has great potential to optimize patient care and simplify logistics for our providers.
Dr. Sarah Mann Wins Abstract Prize at DOM Research Day
-2020.jpeg?sfvrsn=76357cba_0&MaxWidth=137&MaxHeight=137&ScaleUp=false&Quality=High&Method=ResizeFitToAreaArguments&Signature=BA42727F674D40CA5F0453212A156DDA164871BC) Dr.
Mann's award-winning abstract is entitled "Lower Cumulative Antiretroviral Exposure in People Living with HIV and Diabetes." Tenofovir diphosphate (TFV-DP) in dried blood spots (DBS) is a novel pharmacologic measure of cumulative ART adherence
predictive of viral suppression and future viremia. Her findings, also published in J AIDS, revealed that patients who have diabetes mellitus have 25% lower concentrations of TFV-DP in DBS compared to those without diabetes.
Dr.
Mann's award-winning abstract is entitled "Lower Cumulative Antiretroviral Exposure in People Living with HIV and Diabetes." Tenofovir diphosphate (TFV-DP) in dried blood spots (DBS) is a novel pharmacologic measure of cumulative ART adherence
predictive of viral suppression and future viremia. Her findings, also published in J AIDS, revealed that patients who have diabetes mellitus have 25% lower concentrations of TFV-DP in DBS compared to those without diabetes.
Dr. Lakshmi Chauhan receives the EXCCEL Outstanding Clinical Work During COVID Times Award
 This
Department of Medicine award is given to those who have gone above and beyond during the COVID-19 pandemic. Dr. Chauhan has worked tirelessly and with much skill and wisdom to manage our division's response. Her efforts have included but are not
limited to enabling and organizing two new ID services, formulating our treatment guidelines, participating in clinical trials, advising the University of Colorado Hospital, and seeing many extra patients herself. This is an exceptionally well-deserved
award.
This
Department of Medicine award is given to those who have gone above and beyond during the COVID-19 pandemic. Dr. Chauhan has worked tirelessly and with much skill and wisdom to manage our division's response. Her efforts have included but are not
limited to enabling and organizing two new ID services, formulating our treatment guidelines, participating in clinical trials, advising the University of Colorado Hospital, and seeing many extra patients herself. This is an exceptionally well-deserved
award.
ID Division Researchers Find Protein That Helps HIV-1 Navigate Through the Cell
 Mamuka
Kvaratskelia, PhD and colleagues have recently published in Nature Microbiology, their discovery that a cytoplasmic protein, Sec24C, helps the HIV-1 core to maintain
its integrity to successfully reach the nucleus. More can be read about their research here.
Mamuka
Kvaratskelia, PhD and colleagues have recently published in Nature Microbiology, their discovery that a cytoplasmic protein, Sec24C, helps the HIV-1 core to maintain
its integrity to successfully reach the nucleus. More can be read about their research here.
Congratulations to Dr. Michelle Haas for receiving the 2021 Chase Faculty Community Service Award
 This
singular distinction is awarded for an outstanding record of community-centered scholarship, outreach, and service, especially for those who experience adversity. A nominator wrote: “Her passion for equity and social justice has led her
to seek opportunities to help people in our community most in need. For many years she has provided pro bono exams for people seeking asylum. Originally, she would conduct exams after hours in the Denver Metro Tuberculosis clinic. Recognizing
that this was not optimal, she worked with other physician leaders at Denver Health to found the Denver Health Human Rights Clinic…providing complete support for patients and their families including connecting people with legal support
if needed.”
This
singular distinction is awarded for an outstanding record of community-centered scholarship, outreach, and service, especially for those who experience adversity. A nominator wrote: “Her passion for equity and social justice has led her
to seek opportunities to help people in our community most in need. For many years she has provided pro bono exams for people seeking asylum. Originally, she would conduct exams after hours in the Denver Metro Tuberculosis clinic. Recognizing
that this was not optimal, she worked with other physician leaders at Denver Health to found the Denver Health Human Rights Clinic…providing complete support for patients and their families including connecting people with legal support
if needed.”
Variants Arising: Dr. Eric Poeschla, Professor of Medicine, spoke about the emerging SARS-CoV-2 variants in a 50 minute Grand Rounds Presentation on March 10, 2021.
His talk was entitled "Emerging SARS-CoV-2 Variants: Implications for the Pandemic, the Vaccines and our Patients." He reviewed the viral properties of the variants and their epidemiological origins and behaviors inside and outside the U.S. He also discussed pathogenic features, evidence for immune evasion and likely impacts on vaccines and treatments. A recording of the full talk is available here. Recordings of previous town halls hosted by the Department of Medicine are available here.
Drs. Katharine Frasca and Brian Montague to lead the I.D. Fellowship Training Program
 In
July 2021 Physician Educator Dr. Frasca will take on the Program Director role, with Dr. Brian Montague continuing as an Associate Program Director. We look forward to their leadership and extend many thanks to Carlos Franco-Paredes for his excellent
stewardship these past few years and to Dave Beckham and Kristine Erlandson before that. Thanks also to Kelly Rico for her able service as our Education Administrator.
In
July 2021 Physician Educator Dr. Frasca will take on the Program Director role, with Dr. Brian Montague continuing as an Associate Program Director. We look forward to their leadership and extend many thanks to Carlos Franco-Paredes for his excellent
stewardship these past few years and to Dave Beckham and Kristine Erlandson before that. Thanks also to Kelly Rico for her able service as our Education Administrator.
Kvaratskhelia Lab Discovers a Human Protein That Regulates the HIV-1 Life Cycle
 Virologist
Mamuka Kvaratskhelia, Ph.D. and colleagues in the Division of Infectious Diseases have published in Nature Microbiology their discovery that a human cellular protein – Sec24c – critically regulates HIV-1. Sec24c, binds to the outer shell (capsid core) of an incoming virus and is necessary for proper infectivity. First authors are Stephanie Rebensburg,
PhD and Guochao Wei, PhD. Other collaborators included the Melikyan, Poeschla, and Kewalramani laboratories. Understanding the dependency of HIV-1 on this protein may have implications for therapeutic intervention. Notably the discovery follows
on their recent report in Science on an ultra-potent new antiviral drug that also binds to a similar region on the incoming capsid.
Virologist
Mamuka Kvaratskhelia, Ph.D. and colleagues in the Division of Infectious Diseases have published in Nature Microbiology their discovery that a human cellular protein – Sec24c – critically regulates HIV-1. Sec24c, binds to the outer shell (capsid core) of an incoming virus and is necessary for proper infectivity. First authors are Stephanie Rebensburg,
PhD and Guochao Wei, PhD. Other collaborators included the Melikyan, Poeschla, and Kewalramani laboratories. Understanding the dependency of HIV-1 on this protein may have implications for therapeutic intervention. Notably the discovery follows
on their recent report in Science on an ultra-potent new antiviral drug that also binds to a similar region on the incoming capsid.
Dr. Rowan is Associate Director of the Mentored Scholarly Activity Program
Sarah Rowan has been selected for the position of Associate Director of the Mentored Scholarly Activity Program for the University of Colorado School of Medicine. The MSA program is designed to foster self-directed, life-long learning. Students are required to identify and work with a mentor to design and implement a scholarly project. This longitudinal program culminates with students completing a mentored scholarly project, written manuscript, poster, and oral presentation. Sarah will supervise the epidemiology, community, and public health branch of the program. If you are in the Division of Infectious Diseases, expect to hear from Sarah soon about mentoring students and judging the oral presentations.
Drs. Lakshmi Chauhan and Steven Johnson spoke in a DOM Town Hall on "COVID-19 Treatment" Where are We Now?"
 A
recording of the full talk is available here. Recordings of previous town halls hosted by the Department of Medicine are available here.
A
recording of the full talk is available here. Recordings of previous town halls hosted by the Department of Medicine are available here.
Dr. Kristine Erlandson discusses new study for COVID-19 survivors on CU on the Air
 Dr.
Erlandson recently went on the CU on the Air podcast to discuss her work as co-PI on the AFTER Study - a new research study actively recruiting COVID-19 survivors to explore how different personalized physical therapies aid in recovery from the illness. More information can be found at the study website.
Dr.
Erlandson recently went on the CU on the Air podcast to discuss her work as co-PI on the AFTER Study - a new research study actively recruiting COVID-19 survivors to explore how different personalized physical therapies aid in recovery from the illness. More information can be found at the study website.
Dr. Beckham spoke in a Town Hall on monoclonal antibody and convalescent plasma therapies for COVID-19
A recording of Dr. Beckham's full talk is available here. Recordings of previous town halls hosted by the Department of Medicine are available here.
January 18, 2021. The Division honors the legacy of Martin Luther King, Jr.
 “We
have also come to this hallowed spot to remind America of the fierce urgency of now…. I have a dream that one day this nation will rise up and live out the true meaning of its creed…”
“We
have also come to this hallowed spot to remind America of the fierce urgency of now…. I have a dream that one day this nation will rise up and live out the true meaning of its creed…”
Dr. Poeschla spoke in a January 13 campus presentation about the new SARS-CoV-2 variants
 The
full talk, titled "Implications of Genetic Variants of SARS-CoV-2: The Worrying Prospect of a New Pandemic Phase", can be viewed here.
The
full talk, titled "Implications of Genetic Variants of SARS-CoV-2: The Worrying Prospect of a New Pandemic Phase", can be viewed here.
Treating Invasive Mucormycosis
 Invasive
mucormycosis (IM) is a dire infectious complication in immunocompromised people. ID pharmacists Matt Miller and Kyle Molina and Transplant ID physician Maheen Abidi led a multi-center study that showed survival in hematopoietic stem cell recipients with this opportunistic mold infection continues to be poor, but suggested potential benefits of combined treatment -- amphotericin, 3rd generation azoles, and surgical excision -- that
should be prospectively studied further.
Invasive
mucormycosis (IM) is a dire infectious complication in immunocompromised people. ID pharmacists Matt Miller and Kyle Molina and Transplant ID physician Maheen Abidi led a multi-center study that showed survival in hematopoietic stem cell recipients with this opportunistic mold infection continues to be poor, but suggested potential benefits of combined treatment -- amphotericin, 3rd generation azoles, and surgical excision -- that
should be prospectively studied further.
Vaccinations Begin
 SARS-CoV-2
vaccines are now being administered to frontline health care workers on the Anschutz Medical Campus, as well as at Denver Health and the VA Medical Center. Mutiple Division members continue to take care of COVID-19 patients across the city and
have participated both in vaccine science and in enabling the local implementation of the historic national vaccine campaign. Thomas Campbell, MD was featured in the most recent episode of the CU on the Air podcast,
discussing clinical trials of potential SARS-CoV-2 vaccines, with special attention to the Anschutz Medical Campus participation in the Moderna trial which has now received FDA emergency use authorization along with the Pfizer-BioNTech vaccine.
He said that collaboration by many was the key to the success of this effort, noting that the Colorado Clinical and Translational Sciences Institute offered important structure and that UCHealth’s electronic health records made it easier
to identify volunteers to participate in the trial. “There is light at the end of tunnel" he said. It’s been less than 12 months since this illness was first detected in humans and in less than 12 months we now have two vaccines
that have proven to be highly efficacious and that’s unheard of.”
SARS-CoV-2
vaccines are now being administered to frontline health care workers on the Anschutz Medical Campus, as well as at Denver Health and the VA Medical Center. Mutiple Division members continue to take care of COVID-19 patients across the city and
have participated both in vaccine science and in enabling the local implementation of the historic national vaccine campaign. Thomas Campbell, MD was featured in the most recent episode of the CU on the Air podcast,
discussing clinical trials of potential SARS-CoV-2 vaccines, with special attention to the Anschutz Medical Campus participation in the Moderna trial which has now received FDA emergency use authorization along with the Pfizer-BioNTech vaccine.
He said that collaboration by many was the key to the success of this effort, noting that the Colorado Clinical and Translational Sciences Institute offered important structure and that UCHealth’s electronic health records made it easier
to identify volunteers to participate in the trial. “There is light at the end of tunnel" he said. It’s been less than 12 months since this illness was first detected in humans and in less than 12 months we now have two vaccines
that have proven to be highly efficacious and that’s unheard of.”
Dr. Mamuka Kvaratskhelia and Colleagues Publish Groundbreaking HIV Research in Science
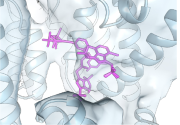 As
we focus on COVID-19, we know that additional pandemics are certain to occur when more viruses cross species barriers from animals to humans. In addition to SARS-CoV-2, no virus illustrates this risk more than HIV-1, for which chimpanzees were
the proximate source about a century ago. Dr. Mamuka Kvaratskhelia, Professor of Medicine in the Division of Infectious Diseases, has now
led a team of researchers in seven U.S. laboratories in uncovering the underlying mechanism of action of a strikingly innovative addition to the HIV therapeutic armamentarium. The research was published in Science on October 16. It concerns the first in class, ultra-potent HIV-1 capsid inhibitor, GS-6207 (Lenacapavir, Gilead). GS-6207 heralds an entirely new way of treating HIV-1. Its remarkable potency and other advantageous features have led to current
clinical trials with very long dosing intervals (six months). Combining molecular biology, virology, structural biology, high resolution imaging of HIV in cells, and an array of biochemical and biophysical methods, the paper reveals the key mechanism:
blocking HIV’s ability to complete infection by hyper-stabilizing and thereby preventing disassembly of the virion capsid shell in infected cells. The work has strong potential to lead to further treatment advances, but it also illuminates
what is still the most mysterious part of the HIV-1 life cycle: the post-entry fate of the virus capsid core as it traverses the cytoplasm and enters the nucleus. Other contributors on our campus were the Asturias and Poeschla laboratories. Mamuka
was also just awarded a new 5-year NIH R01 grant to take this work forward.
As
we focus on COVID-19, we know that additional pandemics are certain to occur when more viruses cross species barriers from animals to humans. In addition to SARS-CoV-2, no virus illustrates this risk more than HIV-1, for which chimpanzees were
the proximate source about a century ago. Dr. Mamuka Kvaratskhelia, Professor of Medicine in the Division of Infectious Diseases, has now
led a team of researchers in seven U.S. laboratories in uncovering the underlying mechanism of action of a strikingly innovative addition to the HIV therapeutic armamentarium. The research was published in Science on October 16. It concerns the first in class, ultra-potent HIV-1 capsid inhibitor, GS-6207 (Lenacapavir, Gilead). GS-6207 heralds an entirely new way of treating HIV-1. Its remarkable potency and other advantageous features have led to current
clinical trials with very long dosing intervals (six months). Combining molecular biology, virology, structural biology, high resolution imaging of HIV in cells, and an array of biochemical and biophysical methods, the paper reveals the key mechanism:
blocking HIV’s ability to complete infection by hyper-stabilizing and thereby preventing disassembly of the virion capsid shell in infected cells. The work has strong potential to lead to further treatment advances, but it also illuminates
what is still the most mysterious part of the HIV-1 life cycle: the post-entry fate of the virus capsid core as it traverses the cytoplasm and enters the nucleus. Other contributors on our campus were the Asturias and Poeschla laboratories. Mamuka
was also just awarded a new 5-year NIH R01 grant to take this work forward.
Dr. Franco-Paredes Awarded 14th Annual Faculty Professionalism Award.
Carlos Franco-Paredes MD, Associate Professor of Medicine, is a recipient of the 14th Annual Faculty Professionalism Award. The Faculty Professionalism Award recognizes a School of Medicine faculty member who has served as a role model for professionalism as defined in the School of Medicine Rules. From the nomination letter: “Carlos advocates for the right thing both within and outside our institution, taking a stand, even when unpopular, to make sure our we are all consistently honoring the core traditions of the profession of medicine.”
Katherine Frasca and Donna McGregor Lead New Virtual TelePrEP/HIV Prevention Program
 UCHealth
has launched a new service, the TelePrEP/HIV Prevention Program. This entirely virtual service allows at-risk people – especially in rural and underserved areas of the state – to confidentially receive medical care for HIV prevention
from trained medical personnel via their computers, smart phones, and tablets. This program is an extension of the existing in-person PrEP Clinic at the Infectious Diseases Group Practice at UCHealth University of Colorado Hospital. Read more at UCHealth Today.
UCHealth
has launched a new service, the TelePrEP/HIV Prevention Program. This entirely virtual service allows at-risk people – especially in rural and underserved areas of the state – to confidentially receive medical care for HIV prevention
from trained medical personnel via their computers, smart phones, and tablets. This program is an extension of the existing in-person PrEP Clinic at the Infectious Diseases Group Practice at UCHealth University of Colorado Hospital. Read more at UCHealth Today.
Santiago and Wilson Labs Decipher Functional Differences Between the Antiviral Interferons
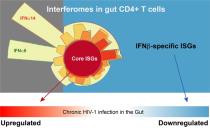 Early
during virus infection, our bodies produce Interferons (IFNs). These antiviral agents are highly diverse, with 12 distinct IFNa subtypes and IFNb being the most highly expressed. Of these, only two, IFNa2 and IFNb, are approved for clinical use,
and in fact are being tested against COVID-19 in ongoing clinical trials. However, Interferons need to be administered with care, as
they cause adverse effects. In PLOS Pathogens, a team led by Drs. Mario Santiago and Cara Wilson now report that IFNa2 is not the most potent antiviral interferon against HIV-1. In a critical target, helper T cells in the gut, IFNa8, IFNa14 and IFNb inhibited
HIV-1 more than IFNa2. Using unbiased transcriptomics, the team then showed that distinct IFNa subtypes and IFNb triggered common and unique gene sets and cellular pathways, suggesting that these diverse Interferons have both redundant and nonredundant
functions. Specifically, IFNb altered 3-times more genes than any IFNa subtype. Interestingly, in the gut of persons with chronic HIV-1 infection, IFNb, but not IFNa, was induced. Genes specifically induced by IFNb were decreased during HIV-1
infection and altered pathways that could promote inflammation and depletion of CD4 T cells, both critical features of AIDS. The work suggests that we should not limit ourselves to the 2 clinically available Interferons to combat viral epidemics
and pandemics; evolution has given us a diverse range of antiviral Interferons to choose and improve upon.
Early
during virus infection, our bodies produce Interferons (IFNs). These antiviral agents are highly diverse, with 12 distinct IFNa subtypes and IFNb being the most highly expressed. Of these, only two, IFNa2 and IFNb, are approved for clinical use,
and in fact are being tested against COVID-19 in ongoing clinical trials. However, Interferons need to be administered with care, as
they cause adverse effects. In PLOS Pathogens, a team led by Drs. Mario Santiago and Cara Wilson now report that IFNa2 is not the most potent antiviral interferon against HIV-1. In a critical target, helper T cells in the gut, IFNa8, IFNa14 and IFNb inhibited
HIV-1 more than IFNa2. Using unbiased transcriptomics, the team then showed that distinct IFNa subtypes and IFNb triggered common and unique gene sets and cellular pathways, suggesting that these diverse Interferons have both redundant and nonredundant
functions. Specifically, IFNb altered 3-times more genes than any IFNa subtype. Interestingly, in the gut of persons with chronic HIV-1 infection, IFNb, but not IFNa, was induced. Genes specifically induced by IFNb were decreased during HIV-1
infection and altered pathways that could promote inflammation and depletion of CD4 T cells, both critical features of AIDS. The work suggests that we should not limit ourselves to the 2 clinically available Interferons to combat viral epidemics
and pandemics; evolution has given us a diverse range of antiviral Interferons to choose and improve upon.
Understanding How Bats are Recurrent Sources of Lethal Human Viruses
 Bats have been primary reservoirs for multiple lethal human viral pathogens, such as SARS, MERS, rabies, Henipa viruses, and most recently, SARS-CoV-2. The probability that further zoonoses will emerge from them is high and the COVID-19 pandemic
suggests that bat innate immune systems are insufficiently characterized relative to the medical importance of these mammals. Restriction factors are main innate immune effectors, limit viral host switching/emergence, and exert strong selection
pressure when it occurs. HIV-1 exemplifies how retroviruses can also be severe pathogens when they cross species barriers, and bats harbor many endogenous and also at least one exogenous retrovirus. The Poeschla lab has now identified and characterized
a retroviral restriction in bats. Working with colleagues in Singapore and Australia, they studied the large bat Pteropus alecto, which is the reservoir species for Nipah virus.
Primate lentiviruses are specifically restricted while nonprimate lentiviruses are entirely unrestricted. The particular retroviral restriction pattern has singular features, but is dependent on viral capsid interactions with cyclophilin A, a
cellular protein known to complexly regulate HIV and SIV replication, including restriction.
Bats have been primary reservoirs for multiple lethal human viral pathogens, such as SARS, MERS, rabies, Henipa viruses, and most recently, SARS-CoV-2. The probability that further zoonoses will emerge from them is high and the COVID-19 pandemic
suggests that bat innate immune systems are insufficiently characterized relative to the medical importance of these mammals. Restriction factors are main innate immune effectors, limit viral host switching/emergence, and exert strong selection
pressure when it occurs. HIV-1 exemplifies how retroviruses can also be severe pathogens when they cross species barriers, and bats harbor many endogenous and also at least one exogenous retrovirus. The Poeschla lab has now identified and characterized
a retroviral restriction in bats. Working with colleagues in Singapore and Australia, they studied the large bat Pteropus alecto, which is the reservoir species for Nipah virus.
Primate lentiviruses are specifically restricted while nonprimate lentiviruses are entirely unrestricted. The particular retroviral restriction pattern has singular features, but is dependent on viral capsid interactions with cyclophilin A, a
cellular protein known to complexly regulate HIV and SIV replication, including restriction.
Women of Color on the Front Lines: Portraits of Unsung Heroes

Dr. Sarah Rowan was featured in CU Medicine Today in an article about her project, Women of Color on the front lines. Artworks by her and fellow artists have been turned into an online gallery that show the strength and determination of health care providers and the creativity and talent of the artists. Dr. Rowan has long painted portraits to relax but in the midst of the pandemic, her hobby took on newfound importance, and prompted her to find a way to celebrate an overlooked community of frontline workers emerging during the crisis. She and her fellow artists seek to honor all health care workers who are on the front lines of the health care response. To raise the profile of women of color, she asked physician friends to send selfies so that she could make portraits. Those friends contacted other friends and within days, Rowan had 150 photos from physicians across the country and has attracted national attention for the project. Over 75 other artists have signed up.
Protecting detainees from COVID-19
 Dr.
Carlos Franco-Paredes was the subject of a feature article in CU Medicine Today about his work inspecting
county jails, advising state prison leaders, and advocating for safer conditions for people held in immigration detention centers. His activities have been multifaceted, and included traveling coast-to-coast to inspect jails and prisons, serving
as the court-appointed inspector of the Prince George’s County Jail in Maryland, and inspecting facilities in Oakland and for the Los Angeles County jail system. He also has issued advocacy letters used in court hearings seeking to create
safer conditions for those held in custody. Collaborating with the Southern Poverty Law Center, the University of Texas School of Law’s Civil Rights Clinic, and other groups, he has produced declarations on behalf of detainees in Immigration
and Customs Enforcement detention centers. He has been actively publishing in peer-reviewed journals, including The New England Journal of Medicine and the Lancet.
Dr.
Carlos Franco-Paredes was the subject of a feature article in CU Medicine Today about his work inspecting
county jails, advising state prison leaders, and advocating for safer conditions for people held in immigration detention centers. His activities have been multifaceted, and included traveling coast-to-coast to inspect jails and prisons, serving
as the court-appointed inspector of the Prince George’s County Jail in Maryland, and inspecting facilities in Oakland and for the Los Angeles County jail system. He also has issued advocacy letters used in court hearings seeking to create
safer conditions for those held in custody. Collaborating with the Southern Poverty Law Center, the University of Texas School of Law’s Civil Rights Clinic, and other groups, he has produced declarations on behalf of detainees in Immigration
and Customs Enforcement detention centers. He has been actively publishing in peer-reviewed journals, including The New England Journal of Medicine and the Lancet.
Professor Steven Johnson Receives the DOM COVID-19 Pandemic Leadership Response Team Award

This innovator award recognizes three responders in the department who were instrumental during the critical phase of the COVID-19 pandemic in the spring of 2020. Dr. Johnson cared for many COVID-19 patients and contributed on several levels to formulating the division and institutional responses. He helped devise evidence-based COVID-19 treatment guidelines and served on the NIH guidelines panel as well. The award will be presented October 29. Zoom link
Congratulations to Jennifer Doudna (who was at CU Boulder from 1991-1994) and Emmanuelle Charpentier on one of the most deserved Nobel Prizes ever. What a Year. Our ID Division scientists use CRISPR all the time now.

A killer pandemic virus, evidence-based cures from deeply creative basic research, amazing scientists. Perfect for 2020. Perfect for any year's prize.

Dr. Cindy Firnhaber and colleagues in South Africa report the outcome of a trial of HPV vaccination in women with HIV and high-grade cervical dysplasia
Women living with HIV often have larger, high-grade lesions (HSIL) or multifocal lesions resulting in incomplete removal of HSIL. Up to 50% of women living with HIV treated with after treatment with Loop electrosurgical excision procedure (LEEP) had persistent or recurrent HSIL compared to 5-10% of HIV negative. The cervical cancer screening and treatment team at the Helen Joseph Hospital in Johannesburg implemented a double blinded placebo controlled randomized clinical trial in 180 HIV-1 infected women with biopsied proven HSIL. Women received the quadrivalent HPV vaccine at baseline, week 4 and 26 during the study. LEEP was done at week 4. The primary endpoint was a composite of HSIL on cervical histology or cytology at week 26 or week 52, and there were a number of secondary measures. The primary endpoint was not significantly different between the vaccine and placebo arms with cytologic or histologic HSIL. Thus, this study did not support HPV vaccination in this setting. Recurrent HSIL was high despite virologic suppression. This work highlights how earlier and improved access to cervical cancer screening and treatment is necessary to prevent the significant burden of cervical cancer in HIV infected women.
Dr. Andrés Henao-Martinez named Editor-in-Chief of Therapeutic Advances in Infectious Diseases. Andrés describes the focus of the journal and his goals:
 "Therapeutic
Advances in Infectious Disease (TAI) - launched in 2013 - is a peer-reviewed open-access journal with a strong clinical and pharmacological focus. TAI delivers the highest quality peer-reviewed open access original research articles, reviews,
and scholarly comment on pioneering efforts and innovative studies in the medical treatment of infectious diseases. TAI welcomes original research articles across all areas of infectious disease. The journal publishes original research articles
and reviews articles primarily. Original research manuscripts may include laboratory, animal or human/clinical studies – all phases. Letters to the Editor and Case Reports are also considered. The journal is listed in PubMed and indexed
in Web of Science, Emerging Sources Citation Index (ESCI) and Scopus). One of the goals as Editor-in-Chief is to increase the volume of submissions and to index the journal in Thomson Reuters' Science Citation Index Expanded (SCIE)".
"Therapeutic
Advances in Infectious Disease (TAI) - launched in 2013 - is a peer-reviewed open-access journal with a strong clinical and pharmacological focus. TAI delivers the highest quality peer-reviewed open access original research articles, reviews,
and scholarly comment on pioneering efforts and innovative studies in the medical treatment of infectious diseases. TAI welcomes original research articles across all areas of infectious disease. The journal publishes original research articles
and reviews articles primarily. Original research manuscripts may include laboratory, animal or human/clinical studies – all phases. Letters to the Editor and Case Reports are also considered. The journal is listed in PubMed and indexed
in Web of Science, Emerging Sources Citation Index (ESCI) and Scopus). One of the goals as Editor-in-Chief is to increase the volume of submissions and to index the journal in Thomson Reuters' Science Citation Index Expanded (SCIE)".
Prisons, the Cycle of Despair, and COVID-19
The United States has extraordinarily high incarceration rates compared to other major developed countries. SARS-CoV-2 is a particularly destructive addition to a stew of correctional system factors that include extreme sentence durations, disproportionate impacts on racial minorities and other historically disadvantaged populations, resistance to paroling elderly individuals for whom recidivism risks are low, crowding, poor ventilation systems, inadequate preventive measures, lower quality medical care and limited treatment access. In The Lancet Infectious Diseases, multiple ID division members recently joined with The Sentencing Project to review the issues and make recommendations for systematic, rational decarceration policies to reduce morbidity and mortality from COVID-19. Dr. Franco-Paredes also gave Department of Medicine Grand Rounds on September 30 on “The Triumph of Despair: Health Inequities and Structural Racism”.
Dr. Haas and colleagues publish encouraging data on a new latent tuberculosis treatment strategy
Treatment of latent tuberculosis infection (LTBI) with short course regimens is now favored over longer traditional regimens such as daily INH for 9 months. Dr. Michelle Haas and her colleagues (Kaylynn Aiona, Kristine Erlandson and Robert Belknap) have now published their analysis of 2 different short course rifamycin-based LTBI regimens from their recent retrospective cohort study. The study was carried out at the Denver Metro Tuberculosis Clinic. They found that INH-rifapentine self-administered once weekly for 3 months (3HP-SAT) was associated with higher completion rates and fewer adverse events than daily rifampin for 4 (4R) months. Importantly, this finding was also seen among adults aged 50 and older in whom safer options for LTBI treatment are needed. They conclude that expanding 3HP-SAT may enhance tuberculosis prevention in the U.S.
Dr. Kristine Erlandson: 12 primary research papers so far in 2020 (and it’s still only September)
National HIV/AIDS and Aging Awareness Day is September 18. Physician-scientist Kristine Erlandson works on understanding physical function impairments in older adults with HIV and improving physical function and disability with physical activity. This work has expanded to encompass impacts of ART-associated weight gain. Among her numerous grants, her current R01 investigates the impact of statins on physical function and she and a co-PI recently received an R01 to investigate High-intensity Interval Training in older HIV patients. Her work in theses areas are highlighted by the following 2020 publications so far (these are half of the total of 12 this calendar year; see the rest in the Publications window). Congratulations to Kristine!
- The Impact of Moderate or High-Intensity Combined Exercise on Systemic Inflammation among Older Persons with and without HIV. J Inf Dis. 2020 Aug 11.
- Physical Function and Frailty Tools in Mortality Prediction of Middle-Aged Adults with HIV.
JAIDS. 2020 Jul 23.
Physical Function Impairment and Frailty in Middle-Aged People Living With Human Immunodeficiency Virus in the REPRIEVE Trial Ancillary Study PREPARE. J Inf Dis. 2020 Jul 9. - Risk Factors for Weight Gain Following Switch to Integrase Inhibitor-Based Antiretroviral Therapy. Clin Inf Dis. 2020 Feb 26.
- Weight Gain Following Initiation of Antiretroviral Therapy: Risk Factors in Randomized Comparative Clinical Trials. Clin Inf Dis. 2020 Sep 12.
- Antiretroviral therapy initiation is associated with decreased visceral and subcutaneous adipose tissue density in people living with HIV. Clin Inf Dis. 2020 Feb 28.
Women in the IDSA: Progress, Future Opportunities
In a recent commentary, Drs. Shanta Zimmer and Janet Gilsdorf review the history of gender disparities within the Infectious Disease Society of America (IDSA) and describe progress toward
equity as well as next steps to maintain efforts with the goal of achieving healthier outcomes for patients. They note that women have played an increasing role since the formation of the IDSA Women’s Committee in 1992. Later task forces
have emphasized the importance of women and other unrepresented minorities, to the success of IDSA core missions. Ongoing efforts in the Society to maintain the presence of women and their unique talents, experiences, and understandings are
important.
Dr. Castillo-Mancilla’s Work on Quantifying Adherence to ART
Adherence to ART is central to quality HIV care and to the prevention of transmission. Dr. Jose Castillo-Mancilla has recently published a major study of five hundred and twenty-seven persons living with HIV (1150 person-visits).Working with a creative set of analytical methods that measure drug concentrations in dried blood spots,he and his colleagues determined patient characteristics that predict the concentrations of tenofovir diphosphate, the active anabolite to the antiretroviral agent tenofovir. This study complements previous analyses that have established the association of this adherence measure with viral suppression (PMID: 30137238) and its utility as a predictor of future viremia (PMID: 30942881) in PWH. Future research to incorporate these predictors into the interpretation of this ART adherence biomarker, and to establish whether these associations extend to PWH taking tenofovir alafenamide-containing ART are ongoing.
Dr. Esther Benamu Provides Expert Opinion on the Roles of JAK-STAT Inhibitors
JAK-STAT inhibitors are powerful immunosuppressive agents with good uses in inflammatory and autoimmune diseases. They are also being studied intensively around the world for use in treating COVID-19-associated inflammation. Dr. Esther Benamu recently reviewed these drugs, along with complement (C5) inhibitors in Infectious Disease Clinics of North America.
Dr. Henao-Martínez and team publish outcome of an extensive systematic review and meta-analysis on the natural history of Chagas disease.
The study, published in JAMA Open Network, established a clear annual risk of cardiomyopathy among asymptomatic individuals in endemic regions. His team found a yearly rate of cardiomyopathy of approximately 5% among patients with acute Chagas infection and 2% among patients with indeterminate chronic Chagas disease. These findings promise to enforce the urgency to diagnose and treat early patients living with Chagas Disease. CU Anschutz News also covered this study in a recent press release.
Dr. Charles Dinarello and colleagues publish clinical trial results on IL-1 receptor blockade in COVID-19 in the Proceedings of the National Academy of Sciences
Dr. Dinarello discovered IL-1 as a key mediator of fever and he has gone on to develop therapeutics that block this important cytokine. Now he and colleagues in France report in PNAS that
anakinra, an IL-1 receptor antagonist, can ameliorate destructive hyper-inflammation in COVID-19.
Drs. Henao-Martínez and Franco-Paredes provide an important perspective on racial inequity and COVID19 in the New England Journal of Medicine
Andrés F. Henao-Martínez, MD and Carlos Franco-Paredes, MD, MPH, are co-authors of a perspective article, “Racial Disproportionality in Covid Clinical Trials,” published last Tuesday by The New England Journal of Medicine. Andrés, Carlos, and their co-authors call out the underrepresentation of minority groups in COVID-19 clinical trials, and in some cases the failure of some studies to disclose racial and ethnic data. “It is alarming that long-standing racial health disparities have been extended to Covid-19 clinical trials when racial and ethnic minority groups have so much to gain from this research, including the opportunity to receive lifesaving treatment,” the authors write.
Dr. Thomas Campbell appointed Chief Clinical Research Officer for UCH Health and Associate Dean of Adult Health Research
Thomas Campbell, MD, Professor of Medicine in the ID Division, has been named Chief Clinical Research Officer for UCHealth and Associate Dean of Adult Health Research. Tom has abundant experience with clinical trials, most recently for COVID-19 interventions, and is the site leader of the Colorado ACTU. He will be responsible for assuring an effective environment for conducting clinical research that complies with federal and state regulatory requirements. The position will foster infrastructure, processes, informatics and analytics to promote high quality UCH and University of Colorado clinical research. Tom succeeds Thomas Flaig, MD, professor of medicine in the Division of Medical Oncology, who was named the University’s Vice Chancellor for Research earlier this year. The division is delighted to see him take on this important role.
Supporting Dr. Fauci
The ID Division stands foursquare with Dean Reilly in his July 20th statement of principle on Dr. Anthony Fauci
and reiterates his call for commitment to science in the COVID-19 crisis and in all other infectious disease policy:
"The number of cases of COVID-19 has been rising significantly across the country and, while the numbers in Colorado have not been increasing as quickly as in other places, we have seen cases here trending upward. The trajectory is a cause for concern and a reminder
that we must remain diligent in our efforts to limit the spread of the coronavirus. It is also clear that willful ignorance and persistent efforts to divide us from one another are not solving the problem. At the Anschutz Medical Campus, we
are committed to the pursuit of evidence, the gathering of data, and the application of that knowledge to lead us to improved understanding of human health and better care for all. That is why the disparagement of Anthony Fauci, MD, director
of the National Institute of Allergy and Infectious Diseases, is so alarming. He is one of our country’s leading champions of pursuing facts for the common good, and he has come under attack recently for doing his work with clear-eyed
purpose.
"With those attacks in mind, I encourage you to read a letter released last Tuesday, by Howard Bauchner, MD, editor in chief of JAMA and the JAMA Network,
stating in part: “As we have learned the coronavirus does not respect state lines – Maine or Alabama, or political parties – Republican or Democrat. The undermining of science – and the unprecedented attacks on scientists
and public health officials – risk lives in every corner of our country. . . . So to all who are reading this – wherever you live and whatever your political affiliation – please wash your hands, keep your distance from others
when appropriate, wear your masks, and please join me in showing respect for Dr. Anthony Fauci and his many colleagues at the NIH, CDC, and throughout the country who are our best hope in these challenging times.”
"It is disheartening
that such a plea needs to be made during the most widespread public health crisis of our lives, but Dr. Bauchner’s message is clear: science matters. You and your colleagues at the CU School of Medicine are also among those professionals
who are our best hope to get through these trying times. We must reject distractions, continue to guard against falsehoods, and remain focused on our common purpose: conquering the coronavirus as soon as possible so that we can pursue all
the other work on this campus that matters. The work you’re doing is too important to be discouraged or diverted. Thank you for your extraordinary efforts to improve our health and safety."
Dr. Katherine Frasca Assumes Associate Fellowship Program Director Role
Dr. Katherine Frasca starts today as Associate Program Director (APD) of the ID Fellowship Program. Katherine will take over Dr. Kristine Erlandson’s role. We welcome Katherine and express our deepest gratitude to Kristine for her many contributions to the training and mentorship of multiple generations of infectious disease fellows. Dr. Carlos Franco-Paredes is Program Director (PD) and Katherine and Dr. Brian Montague are the two APDs. Katherine brings a wealth of clinical & educational experience to our program. She has a stellar record in Education and the Scholarship of Teaching. She is locally and regionally recognized as a leader in medical education on HIV prevention. During the first year of her promotion to assistant professor, she was one of four recipients of the prestigious Program Academic Clinician Educator (PACE) grant, which provides scholarly support for medical education research. During that same year, she also completed the Teaching Scholars Program, learning skills in curriculum development, evaluation and medical education research. In assembling both of these programs, she has created and directed a comprehensive clinical and educational program on HIV prevention. She has developed a novel virtual curriculum on HIV pre-exposure prophylaxis (PrEP). Additionally, Katherine has been coordinating the schedule and teaching activities for the Fellows Clinic at Anschutz Medical Center Infectious Diseases Division since 2017.
Sarah Rowan MD and Whitney Starr NP, MSN Promoted to Associate Professors
The Division is pleased to announce that Sarah Rowan and Whitney Starr have each been promoted to Associate Professor. We congratulate them for their well-deserved promotions and recognize our good fortune in having such superb, dedicated faculty. Among their many accomplishments, both Sarah and Whitney are key contributors to the division’s deep expertise in chronic viral diseases. Each has been very active in HIV medicine, and Sarah also in the area of HCV. They have been active since February in the division’s vigorous response to COVID-19 as well.
Dr. Martin Krsak Selected in July 2020 to be the Featured Provider for the CU Doctors Web Page.
Recruited from the Tufts University Division of Infectious Diseases in 2017, Dr. Krsak has been active in numerous clinical and scholarly activities related to the COVID-19 efforts of our medical school. The CU Doctors homepage can be found here.
Campus Participates in COVID-19 Moderna mRNA SARS-CoV-2 Vaccine Trial Under Leadership of PI Tom Campbell
“Our site here at University of Colorado Hospital is part of a nationwide network called the COVID Prevention Network, which is set up so that it has a cohort of sites that are available to sequentially enroll into multiple vaccine studies,” said Dr. Thomas Campbell, an infectious disease physician at the CU School of Medicine and University of Colorado Hospital. “If it works, the Moderna vaccine could be a real game-changer for the pandemic.” Watch the full interview with Dr. Campbell featured in the UCHealth Today article covering the vaccine trial launch.
James Colbert, MD Awarded the Golden Apple Teaching Award
The award was announced by graduating fellows at their virtual graduation party. Fond tributes were made by many faculty for graduating fellows Angela Budgin, Shelly Kon, Sarah Mann, and Sias Scherger. The fellows cited Dr. Colbert’s dedication to teaching and emphasis on understanding evidence-based rationales for testing, diagnosis and therapies.
Sara Rowan, MD Featured in Colorado Public Radio News for her Recent Work on a Creative Portrait Series Honoring Women of Color on the Medical Front Lines
From Dean Reilly’s weekly message July 6, “CPR News featured Sarah Rowan, MD, assistant professor of medicine in the Division of Infectious Diseases, in a recent report about finding a creative and meaningful way to take a break from the non-stop cycle of work our colleagues have been facing this year. Sarah, who practices at Denver Health and is an artist in her free time, was inspired to create art that features women of color who have been providing care in the time of COVID-19. She emailed friends at local hospitals, including Shanta Zimmer, MD, senior associate dean for education, associate dean for diversity and inclusion, and professor of medicine, to ask for selfies that could be turned into portraits, which are now featured on a specially created website, Women of Color on the Front Lines. “I hope that it serves as a visual representation that our society values women and racial diversity in medicine, and their commitment is worth recording with artwork,” Sarah said. “I hope that people feel honored and appreciated. I also feel hopeful that this will inspire young people to go into medicine, particularly young Black people or Latinx people.””
Dr. Charles Dinarello Awarded the 2020 Tang Prize
Dr. Charles Dinarello in the Division of Infectious Diseases has been awarded the 2020 Tang Prize in Biopharmaceutical Sciences. The prize was awarded for “the development of cytokine-targeting
biological therapies for the treatment of inflammatory diseases.” See also the CU Anschutz Today article.
He shares this year’s prize with two colleagues, Marc Feldmann and Tadamitsu Kishimoto. Charles discovered Interleukin-1 and is an author of over 1,000 scientific papers. His work has applications to diverse fields and most recently
his laboratory has been working on treatments for the hyper-inflammatory problems seen in COVID-19. More about the Tang Prize, which is awarded every two years to two to three distinguished scientists, can be found here.
Charles has previously been awarded a University Distinguished Professorship, which is the highest honor that the University of Colorado bestows on its own faculty
members. Congratulations to Dr. Dinarello on this extraordinary recognition and on all his scientific achievements.
The Division Welcomes 4 New ID Fellows
The Division is delighted to welcome four new ID fellows, who started July 1, 2020. They bring to us a wealth of education, experience and talent from diverse backgrounds. Biographies are coming soon to the Education page.
Dr. David Fraulino
David joins us from the University of Connecticut internal medicine residency and is graduate of the University of New England College of Osteopathic Medicine.
Dr. José Henao
Jose joins
us from the University of Minnesota internal medicine residency and is a graduate of the Universidad de Ciencias Medicas Andrés Vesalio Guzmán (UCIMED) Escuela de Medicina, Costa Rica.
Dr. Zachary Shepard
Zachary joins us from the University of Michigan internal medicine residency and is a graduate of the Baylor College of Medicine.
Dr. Lilian Vargas
Lilian joins us from the Houston Methodist Hospital
internal medicine residency and is a graduate of the Universidad Nacional Autónoma de Honduras Facultad de Ciencias Médicas, Honduras.
Read all about Dr. Michelle Barron’s Inspiring Life Story and Career
Dr. Barron is Professor of Medicine in the ID Division and Medical Director of Infection Control and prevention. On January 8, 2020, she emailed her colleagues: “Hello. Happy New Year! Never a dull day in infection prevention. There is a severe respiratory disease due to a novel coronavirus that is causing an outbreak in the Wuhan province of China.” The full article, "A fearless protector: Meet the top infectious disease expert in Colorado", can be found at UCHealth Today. Drs. Barron and Larissa Pisney are the point persons for Infection Control in our main academic hospital, UCH.
HIV Training Grant Awarded
The Division of Infectious Diseases will be home to a new T32 program for postdoctoral training in Antiretroviral Discovery, Evaluation and Application Research (ADEAR). ADEAR will provide postdoctoral scientists with mentored research training under the direction of faculty at the University of Colorado, Colorado State University and the University of Denver who are who engaged in research related to the discovery and evaluation of new antiretroviral drugs or the application of existing antiretrovirals for the treatment and prevention of HIV/AIDS. The program is expected to kick off in July 2020 and will support 3 trainees per year through June 2025. A request for applications will be released in early July.
Dr. Franco-Paredes Interviewed by the New York Times on the Worsening Problem of COVID-19 in Prisons
The full article can be read here.
Drs. Krsak, Henao-Martinez, and Franco-Paredes Advocate in the NEJM for Serological Testing in Correctional Facilities
Their recommendations can be read in full here.
Multiple Division Faculty are Contributing to COVID-19 Clinical Trials Research
Read about our role in developing antiviral medications and working to attenuate the virus's inflammatory response here.
Dr. Katherine Frasca Has Created a COVID-19 TipSheet/Survival Guide Based on Her and Our Other ID Physicians' First-hand Experience
Dr. Frasca recently attended to numerous COVID-19 inpatients and has compiled this very helpful and practical resource which can be found in our COVID-19 document collection on our division's COVID-19 resources page. Stay tuned for expansions and refinements by her and our other physicians of this living document.
Associate Professor David Beckham, MD Has Been at the Forefront of Efforts to Deploy Convalescent Plasma for COVID-19 Patients in Colorado
Dr. Beckham was featured in a recent news report about how researchers and clinicians are working together on our campus to make a serum test available. The University of Colorado Hospital was the first in the state to treat COVID-19 patients with convalescent serum. This work is supported in part by a CCTSI pilot award.
Division Faculty Advocate for Immigrant and Disadvantaged Populations
Dr. Carlos Franco-Paredes works with a national network of physicians dedicated to provide medical care for immigrants under ICE custody. Dr. Michelle Haas has been volunteering in the Human Rights Clinic (HRC) at Denver Health. Janine Young and Jaime Moo-Young lead the HRC. In response to COVID-19, Carlos has actively collaborated with RMAIN, ACLU, Southern Poverty Law Center, and numerous immigration attorneys to promote the release of detained immigrants on humanitarian parole. Implementing interventions such as social distancing and infection prevention is a major challenge in for-profit overcrowded detention centers.
ID Faculty Photo Panel Now Available on ID Division Website
The "Faces of the ID Division" card below provides a photo panel showing our faculty arranged in order of year of appointment to the CU SOM faculty. The 72 faculty distribute as follows: AMC-51, Denver Health-15, Veterans' Affairs-4 (7 counting joint roles), NJH-2. On the AMC (UCH), there are 40 ID clinicians who staff our inpatient and outpatient ID services (32 physicians, 8 APPs). Fourteen of our faculty have laboratory-based programs in Research Complex 2 (RC2).
Weekly Division Case Conferences Have Moved to a Virtual Format
In response to COVID-19, the Division’s weekly Case Conference is now a virtual series that will focus on this new infectious disease and engage the campus and the broader Colorado medical community. Fellows and faculty present and discuss COVID-19 cases and medical students provide a literature review. This is a joint collaboration between CU Anschutz, Denver Health, Colorado IDSA, and ECHO Colorado.
Professor Shanta Zimmer Rolls Out New COVID-19 Course at the CU School of Medicine
Professor Zimmer, Senior Associate Dean for Education, has led a team of educators and students in setting up the COVID-19 Pandemic Response Elective Course in record time. It is also posted at the iCollaborative website of the AAMC.
Professors Eric Poeschla, Steven Johnson, and Thomas Campbell Present COVID-19 Grand Rounds
Their grand rounds [video link] presentation on April 1 gave an overview of epidemiological modeling, origins and properties of SARS-CoV-2, clinical features, and treatment. They were joined by Professor Jonathan Samet from the CU School of Public Health.
Division Activates Additional Inpatient ID Service in Response to COVID-19
On 24 March, the Division activated a 5th inpatient ID service (Green) to meet the needs of COVID-19 patients. The pre-existing services are Gold ID, Blue ID, Ortho-ID and Transplant ID. In addition, faculty are participating in several COVID-19 clinical trials, organizing outpatient follow-up visits, providing updated treatment and monitoring guidelines, and supervising hospital infection control.
We Welcome Five Incoming Faculty Members
The Division is Growing. In July we will be 72 faculty members strong. A fifth inpatient service will soon start at University of Colorado Hospital. We are delighted to officially announce five new ID Division faculty members who will join us
in mid-2020. They collectively bring a wealth of talent, training and diverse experiences to our three-shield missions:
Yiannis Koullias, MD comes to us from the Partners ID fellowship at Harvard Medical School/Brigham
& Women’s Hospital/MGH, with subspecialty training in Transplant ID at Dana-Farber/Brigham and Women’s Cancer Center. He is a graduate of Harvard College, Duke Medical School, and the Brigham’s Internal Medicine Residency
Program. His has broad interests in Transplant ID, including viral and fungal infections in heme-onc/BMT populations.
Sarah Mann, MD joins us from our ID fellowship here at the University of Colorado School of Medicine.
She is a graduate of Cornell University, George Washington University Medical School and the Harbor UCLA internal medicine residency. She has interests in HIV Medicine and works on stewardship of anti-retroviral agents.
Aakriti Pandita, MD joins us from the Infectious Disease Fellowship at Warren Alpert Medical School of Brown University. She is a graduate of the Sher-i-Kashmir Institute of Medical Sciences in Srinagar, India,
and the SUNY Upstate Medical University internal medicine residency. She is jointly appointed with the Division of Hospital Medicine. She is currently working on a meta-analysis of decades-long time trends in Staphylococcus aureus bacteremia.
She also has a strong interest in tuberculosis and advocacy.
Rebecca Rwubusisi MSN, BSN, is our new APP for the Transplant ID (TID) service on the AMC. She is an Acute Care Nurse Practitioner whose valuable experience
includes 15 years of bedside experience as an RN in the Department of Surgery, on the UC Health Inpatient Transplant Unit. She also has medical experience in East Africa and is fluent in Spanish.
Sias Scherger, MD also joins the division from our ID fellowship. He is a graduate of the University of Nebraska, the University of Nebraska College of Medicine and the Wake Forest internal medicine residency. He has interests in transplant ID and is working
on understanding associations between anti-cytokine antibodies and endemic fungal infections.
Responding to COVID-19. The CU Infectious Diseases Division Continues to be Deeply Involved in Institutional Preparations for the Coronavirus Pandemic
Drs. Michelle Barron and Larissa Pisney (University of Colorado Hospital Infection Control and Prevention) are at the head of a multi-faceted campaign to ready our UCH providers and trainees and have been coordinating with state and national authorities. Drs. Mary Bessesen and Heather Young have been performing similar roles at the VA Medical Center and Denver Health. Dr. Brian Montague is involved in managing employee health for both the School of Medicine and UCH. Numerous other ID faculty members have participated in patient care, screening and testing, contingency planning, guidelines preparation, communications and community outreach, scientific discussions, idea generation, and teaching. Division scientists are working on various research aspects of understanding, preventing and treating viral infections. The Infectious Disease Fellows are involved in consulting on COVID-19 issues and they will also be working with the Colorado Dept. of Public Health in the coming month to learn about the role of epidemiologists and about public health policy. The Division website aggregator contains much practical information, both local and international.
Dr. Michelle Barron Speaks at UCHealth Town Hall on COVID-19 Response
Dr. Barron, Medical Director of Infection Control and Prevention, discussed COVID-19 basics, screening and treatment guidelines, and infection control measures. The entire town hall can be watched here.
Drs. Robert Belknap, David Cohn and Randall Reves Participate in Multi-institutional Team to Update Guidelines for Treatment of Latent Tuberculosis.
Their participation is part of the important role that Denver Health ID faculty continue to play in M. tuberculosis treatment and control, in Colorado and internationally. See Sterling et al. in MMWR in "Recent Publications" below for full details of the team's report.
Dr. Lakshmi Chauhan Receives the Outstanding Quality Award at 2nd Annual UCH Quality & Safety Symposium
Dr. Chauhan was awarded for her outpatient stewardship project “Approaches to Decrease Inappropriate Antibiotic use in Acute Respiratory Conditions in a Geriatric Clinic.” She will present her project on March 11, 2020. Her goals are to work with the antimicrobial stewardship team to help expand outpatient stewardship programs to other UCH clinics. Quality improvement projects such as this are important areas for academic contribution and grant funding opportunities in the division.
Dr. Sarah Rowan Discusses Colorado's Ongoing Fight to End HIV with 5280 Magazine.
Dr. Rowan spoke about her work on a local HIV task force to expand testing and treatment of the virus and about other efforts by the Colorado medical community to combat HIV.
Congratulations to Fellowship Program Director Dr. Carlos Franco-Paredes and Education Coordinator Kelly Rico for Highly Positive ACGME Annual Program Review.
ID Fellows Greg Canfield and Sarah Mann Publish a Striking Example of Cutaneous Blastomycosis.
Drs. Canfield and Mann published their results in Clinical Infectious Diseases. The case exhibited numerous interesting features including the classic - and in this case, quite developed - verrucous lesion with raised, sharply demarcated borders.
Dr. Hillary Dunlevy Awarded Annual CU Hospital Physician Medical Staff Award
Rebecca Rwubusisi MSN, BSN, RN, CCTN Joins Our Team as the New APP for Transplant ID Service
Debra Best Joins Our Division as Our New Post-Award Administrator
She will begin her role on Monday, February 3rd, 2020.
Dr. Cara Wilson has been appointed Associate Director of the Medical Scientist Training Program
Dr. Wilson will transition into the director role on July 1, 2020. Our MD-PhD program is a critical linchpin in the education of physician-scientists, allowing top-notch students to obtain their PhD alongside their MD. The program provides tuition as well as an annual stipend.
Dr. Michelle Barron Discusses Infection Prevention with Boulder Daily Camera
Michelle Barron, UCHealth University of Colorado Hospital’s medical director of infection prevention and professor of medicine at CU School of Medicine was recently interviewed by the Daily Camera. She discussed how Boulder County has managed to avoid the worst of a state and nationwide Hepatitis A outbreak.
Dr. Tom Campbell to lead scientific review group on HIV
Dr. Tom Campbell has been nominated to lead the new Section Review Group of the NIH-CDC-HIVMA-/IDSA Guidelines for Prevention and Treatment of Opportunistic Infections in Adults and Adolescents with HIV.
Dr. Kristine Erlandson Announced as Outstanding Early Career Scholar
The University of Colorado Department of Medicine has selected the 2017 recipients for its Outstanding Early Career Scholar Program, HIV/AIDS researcher Kristine Erlandson, MD, and cardiology researcher Kunhua Song, PhD. The program aims to accelerate the careers of promising researchers in the Department of Medicine.