CU Limb Restoration Program - Osseointegration
Osseointegration is an advanced reconstructive surgery technique for amputees that eliminates the need for a traditional prosthesis. Because the implant connects directly with the bone of the residual limb, osseointegration patients regain body awareness and improve their balance and gait.
Osseointegration offers patients a better quality of life and improved function & mobility without the usual socket prosthesis-related issues such as pinching, sweating, muscle weakness, and skin irritation.
Osseointegrated bone-anchored prostheses can be implanted in the humerus (upper arm bone), radius or ulna (forearm bones), femur (thigh bone), or tibia (lower leg bone).
What is Osseointegration
Am I a Candidate for Osseointegration Limb Replacement?
Osseointegration implants are a good option for amputees who are having a poor experience with their current prosthesis or do not want to use a traditional prosthetic leg or arm. Socket prostheses can be difficult for patients with a residual limb that is scarred, short, or wide. Because osseointegrated implants are implanted directly into the remaining bone, the shape of the residual limb does not cause the pain and discomfort patients typically feel with a traditional socket prosthesis.
Patient Evaluation Process
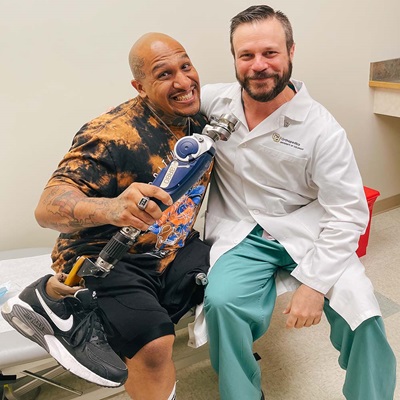
Why choose the University of Colorado Limb Restoration Program?
Dr. Jason Stoneback, Director of the Limb Restoration Program, is one of the few physicians across the globe who has been trained in all osseointegration implant procedures.
Since its founding in 2015, the University of Colorado Limb Restoration Program has been unique in its comprehensive, multidisciplinary approach. All of our patients receive world-class care and personalized attention. Each patient is monitored by our Osseointegration Program Coordinator, who guides patients through the program.
Our team includes a social worker and amputee rehabilitation specialist, as well as physicians specializing in wound care, plastic surgery, foot & ankle care, interventional radiology, endocrinology, rehabilitation medicine, prosthetics, infectious disease, gait analysis, vascular medicine, and musculoskeletal oncology. We are proud to earn our 100% patientsatisfaction rate.
Our Team Members
Osseointegration Physicians

Jason W. Stoneback, MD
Dr. Jason W. Stoneback, Director of the Limb Restoration Program, was one of the first orthopedic surgeons to offer osseointegration surgery in the United States and is widely considered to be one of the best osseointegration surgeons in America. He has performed over 100 successful osseointegration surgeries and is regarded as a world expert in the field. Dr. Stoneback has been a practicing orthopedic surgeon since graduating from the University of Tennessee in 2006 and was trained in both OPRA and press fit osseointegration techniques in Germany and the Netherlands. He strongly believes in the connection between form and function and strives to provide patients with real options – often when all other choices have been exhausted.
Learn more about Dr. Stoneback’s clinical and research work by clicking here.

Danielle Melton, MD
Dr. Danielle Melton, Director of Amputation Medicine and Rehabilitation for the Limb Restoration Program, specializes in the rehabilitation of orthopedic trauma patients. She is a leading medical expert on amputation medicine and osseointegrated amputees and has been selected by her peers as a “Best Doctor in America” every year since 2009. She is the Co-Chair of the Limb Restoration Rehabilitation Group of the American Congress of Rehabilitation Medicine, serves as the Scientific Chair for the Limb Loss and Preservation Registry (a National Institutes of Health/Mayo Clinic initiative), and does research with the Department of Defense’s Major Extremity Trauma Research Consortium (METRC).
Learn more about Dr. Melton’s clinical and research work by clicking here.
Osseointegration News & Video
-
Osseointegration: Nuts and Bolts of OIOpens in a new window
Jan 13, 2026Join leading experts from the University of Colorado Limb Restoration Program—Dr. Jason Stoneback and Dr. Danielle Melton—as they share the latest insights, advancements, and practical knowledge in the field of osseointegration.Opens in a new window Full story -
Restored Limb Puts Cyclist Back in the RaceOpens in a new window
Oct 15, 2025The University of Colorado Anschutz is a world-class academic medical campus at the forefront of transformative science, medicine, education and patient care. The campus encompasses the University of Colorado health professional schools, more than 60 centers and institutes and two nationally ranked independent hospitals - UCHealth University of Colorado Hospital and Children's Hospital Colorado – which see more than two million adult and pediatric patient visits yearly. Innovative, interconnected and highly collaborative, CU Anschutz delivers life-changing treatments, patient care and professional training and conducts world-renowned research.Opens in a new window Full story -

Unique surgery allows Colorado man to represent Team USA in paracycling world championships
Oct 14, 2025AURORA, Colo. — A man from Colorado always hoped one day he'd compete for Team USA, but medical setbacks threatened that dream. A unique surgery performed at CU Anschutz has changed everything for him. "Every time I pull on the USA clothing, it feels really special," said Jason Macom, a paracyclist for Team USA competing in the world championships in Brazil.Full story -

Breaking Away: Restored Limb Lets Cyclist/Amputee Feel Free AgainOpens in a new window
Oct 13, 2025Jason Macom feels most alive when life goes by in a blur. He thrives in the velodrome, a cauldron of speed that rewards endless hours of lung- and leg-busting training, mental focus and fearlessness. But over two spans in the past 15 years, the adrenalized world of track cycling came to an abrupt halt for Macom. The first (2010 to 2015) came after a severe leg injury in a bicycle accident that eventually required an amputation below his knee. The second (2021 to 2024) saw his para-cycling career shelved by painful chafing and bursitis where his residual limb met a traditional socket prosthesis.Opens in a new window Full story -
-bottomley.png?sfvrsn=9b23c8b4_1)
2025 Saving Lives and Limbs Gala Mission MomentOpens in a new window
Apr 28, 2025Meghan Kroyer and Mark (MC) Bottomley, Commerce City, CO. In 2022, Mark was struck by a vehicle while riding his moped.Opens in a new window Full story
OUR LOCATIONS
OUR LOCATIONS
PRACTICE LOCATIONS
CU Limb Restoration Program - University of Colorado Hospital
1635 Aurora Court Anschutz Outpatient Pavilion, 4th floor, Aurora, CO 80045To make an appointment call: 1-844-800-LIMB (5462)
Fax: 720-553-0402
For urgent or emergency transfers, call the Access Center at: (720) 848-2828
E-Mail:
[email protected]
