Research Projects
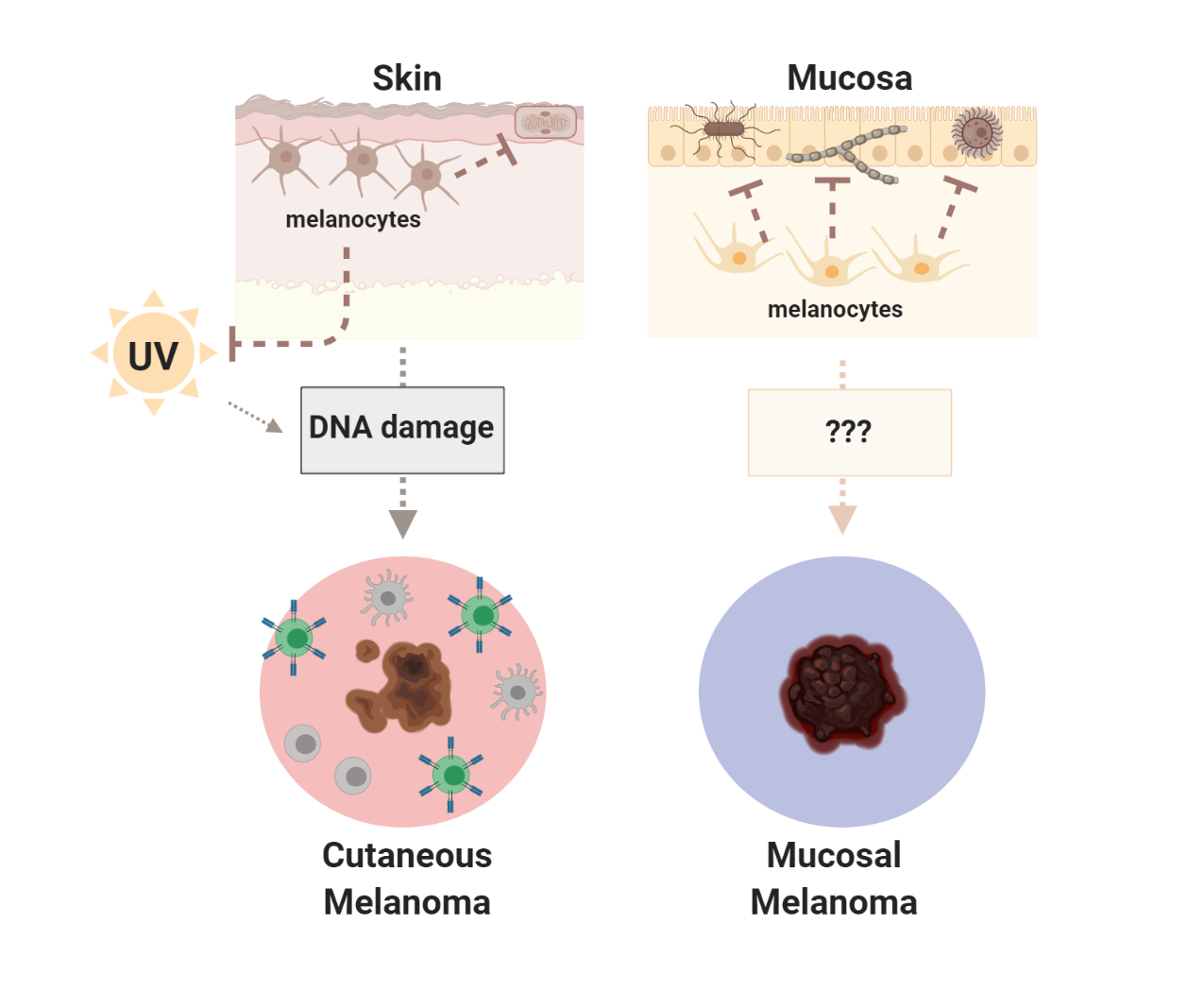
WHY TAKE OUR SURVEY? One of the questions we frequently get asked by patients is "why did I develop mucosal melanoma?" Researchers are working hard to identify possible genetic factors that may underlie mucosal melanoma risk, but WE NEED PATIENTS to anonymously complete surveys and provide us medical history and lifestyle data that researchers have no access to otherwise. Our goal is to learn more about mucosal melanoma risk factors which may ultimately lead to PREVENTION and EARLIER DETECTION.
THE SURVEY: The link above will take you directly to our anonymous patient survey. After you complete the survey, please enter your email address (this will NOT be saved anywhere) so you can be sent your survey ID number and a form to print off and give to your oncologist. PLEASE write your ID number on the form and give to your oncologist so they can anonymously add detailed information about your melanoma and treatments which will be linked to your responses. Your oncologist will NOT be able to see any of your survey responses.
THANK YOU for considering our survey and passing along the link to this webpage to other mucosal melanoma patients!!
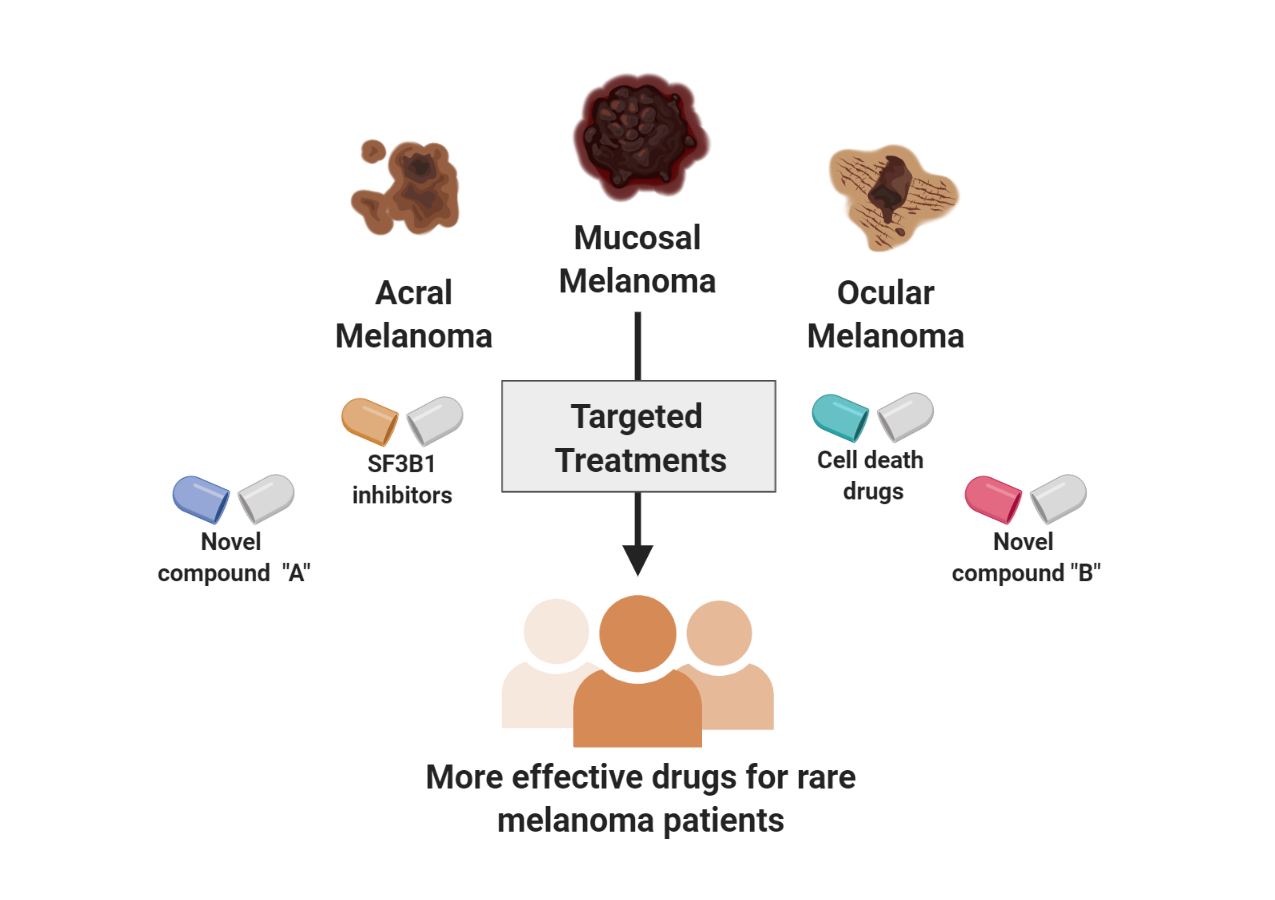
Below are just a few of the rare melanoma focused research projects underway at the Center for Rare Melanomas: