
CHA/PA Program Overview
The three-year, innovative curriculum of the University of Colorado PA program is designed to integrate clinical and basic sciences to prepare graduates with the knowledge, skills, and attitudes to practice medicine as part of the health care team. Graduates practice in all areas of medicine and serve patients of all ages.
The information below pertains to the Colorado Curriculum, which was adopted in 2018 and applies to students graduating in 2021 and beyond.
The Colorado Curriculum is a cutting-edge, learner-centered educational platform designed to foster clinical decision-making and lifelong-learning skills. The curriculum is based on clinical presentations, which mimics how patients present for care and how clinicians practice medicine. For example, during the week of the curriculum focused on the clinical presentation “shortness of breath”, all learning in the basic sciences and clinical medicine is delivered in the context of a patient with shortness of breath.
The Colorado Curriculum consists of two didactic years, with clinical experiences integrated across both years. The third year of the program consists of 10 one-month rotations. The program begins in July with a summer immersion course that includes fundamentals of learning strategies, PA professional roles, wellness and resilience, and clinical topics.
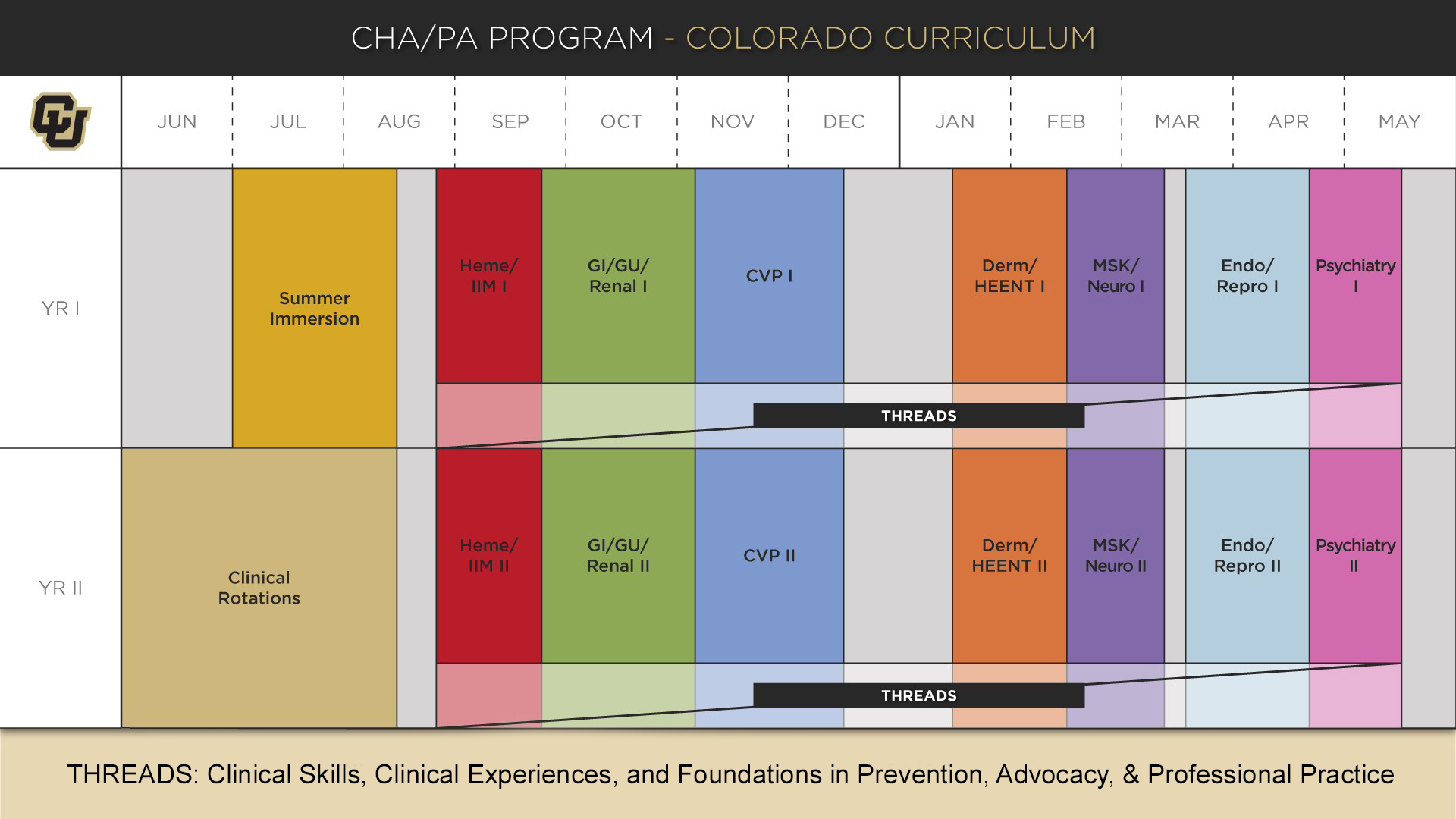
The curriculum is organized into seven system-oriented blocks: Hematology, Infection, Inflammation and Malignancy (Heme/IIM); Gastrointestinal, Genitourinary and Renal (GI/GU/Renal); Cardiovascular and Pulmonary (CVP); Dermatology and Head, Eyes, Ears, Nose and Throat (Derm/HEENT); Musculoskeletal and Neurology (MSK/Neuro); Endocrinology and Reproduction (Endo/Repro); and Psychiatry. The curriculum is an iterative, spiral approach to learning, such that clinical topics which are introduced in the first year are often revisited at a more advanced level in the second year. Each block course integrates basic sciences and clinical medicine by employing the use of small group experiences, case-based learning, standardized patients (SPs), patient simulations, lectures, and collaborative, hands-on sessions. Additionally, students participate in thread courses over both years which provide education in clinical skills, role development, advocacy, patient care for diverse patient populations, wellness and preventive medicine, and early clinical exposures. The thread courses include Clinical Skills, Clinical Experiences, and Foundations in Prevention, Advocacy, and Professional Practice. See the individual course descriptions for further details on course content. An overview of the vision and goals of the Colorado Curriculum are illustrated in this LICENSE document.
Interprofessional Education and Tracks
Educational content is enhanced through the applications of family-centered care, behavioral and psychosocial perspectives as well as social and community initiatives for health and wellness. The program has integrated content in public health, oral health, professionalism, and interprofessional education. Students with a personal area of interest may also have the opportunity to participate in specialized tracks to enhance learning in adult hospitalized patients, pediatric critical and acute care, or rural health.
Clinical Experience and Affiliates
The curriculum includes fully integrated clinical experiences in hospital and community settings. During clinical experiences, students may observe a practitioner's practice, but may also participate in history-taking, physical examination and assessment,
development of a differential diagnosis and clinical decision-making and planning of treatments and interventions. Students work closely with preceptors and other members of the health care team and are evaluated on skills and competencies required
for patient care.
All rotations are scheduled by the Clinical Team based on accreditation standards, program requirements, track requirements, and preceptor/site availability. The Clinical Team is not able to accommodate specific requests for rotations, students will be scheduled in rotations in a variety of settings across multiple disciplines throughout their time in the program.
As a part of the University of Colorado School of Medicine, the faculty of the entire school of medicine and affiliates contribute greatly to the quality of the learning experiences provided at the CHA/PA Program. Affiliations with the University of Colorado Hospital, Children’s Hospital Colorado, and Denver Health and Hospitals in addition to community clinics, provide a network of clinical experiences to enhance the training of students. The faculty within the departments of Pediatrics, Family Medicine, Internal Medicine, Surgery, and others regularly participate in both classroom and clinical training of the CHA/PA Program students.
Degree
The University of Colorado PA Program has gained national recognition for its curriculum in primary care medicine. The Program confers a Professional Master’s Degree (MPAS). In accordance with the mission of the program, the CHA/PA Program curriculum provides comprehensive physician assistant education in primary medical care with additional training in pediatrics and disadvantaged, at-risk and medically underserved populations. There are specific requirements that all students must complete to receive the MPAS degree from our fully accredited PA Program. Graduates are well prepared to perform in primary care practice with patients across the lifespan. Historically our students have performed above the national average in score and passing rate on the National Commission on Certification of Physician Assistants (NCCPA) examinations.
Graduation and awarding of the Masters of Physician Assistant Studies is based upon the following requirements:
- Successful completion of all coursework and rotations of the University of Colorado PA Program
- Exhibiting professionalism throughout the course of study
- Successful completion of the Comprehensive Clinical Knowledge and Clinical Skills Examinations
In the first year of the program, student learning utilizes a variety of approaches including small group experiences, lectures, interprofessional sessions, laboratories and clinical experiences. Hands-on learning is gained through clinical skills and laboratory sessions in addition to direct clinical experience. Early clinical experiences begin in the 3rd semester to allow students to start practicing the skills they are learning in the classroom. Students must pass all first-year courses in order to be promoted to second year. Click here to see a list of the courses required for CHA/PA Students.
The third year (June through May) consists of ten, one-month long rotations and a one-month vacation that can be used to complete professional development modules, Capstone requirements, and self-care activities. The required rotations and elective rotations are dependent on the student’s track. All students, regardless of track, must complete one-month in either an out of metro area or medically underserved site.
Students complete a capstone project during year three, returning to campus during the final month of the program to present their topic as part of the Clinical Connections courses. The project represents a culmination of student progress through the program and allows students to identify a clinical case that illustrates a practice-based and/or systems-based approach to care.
Students are required to pass all 3rd Year clinical rotations, the requirements for Clinical Connections, as well as the 3rd Year comprehensive written (knowledge-based) and clinical (practice-based) exams consisting of knowledge and practical standardized patient exams in order to be eligible for graduation from the program.
Traditional Track — 35 Hours (Courses Are Subject to Change)
| Months | Type of Rotation |
| 1 month | Primary Care I - Ambulatory Pediatrics (MPAS 6930) |
| 1 month | Pediatric Specialty - Newborn Nursery (MPAS 6920) or Peds sub-specialty (MPAS 6936) or Adolescent Medicine (MPAS 6938) |
| 1 month | Inpatient Medicine - Pediatric (MPAS 6932) or Adult (MPAS 6942) |
| 1 month | Primary Care II - Family Medicine (MPAS 6940) |
| 1 month | Emergency Medicine - MPAS 6948 |
| 1 month | Primary Care III - Women's Health (MPAS 6947) |
| 1 month | Surgery - MPAS 6905 |
| 1 month | Primary Care IV - Internal Medicine (MPAS 6974) |
| 2 months | Electives - Pediatric (MPAS 6936) or Adult (MPAS 6970) |
| 1 month | Vacation |
| Fall Semester | Clinical Connections I - MPAS 6978 |
| Spring Semester | Clinical Connections II (with Capstone) - MPAS 6979 |
Pediatric Critical & Acute Care (Courses Are Subject to Change)
| Months | Type of Rotation |
| 1 month | Primary Care I - Ambulatory Pediatrics (MPAS 6930) |
| 1 month | Pediatric Specialty - Newborn Nursery (MPAS 6920) or Peds sub-specialty (MPAS 6936) or Adolescent Medicine (MPAS 6938) |
| 1 month | Inpatient Pediatric Medicine - MPAS 6932 |
| 1 month | Primary Care II - Family Medicine (MPAS 6940) |
| 1 month | Surgery - MPAS 6905 |
| 1 month | Emergency Medicine - MPAS 6948 |
| 1 month | Primary Care III - Women's Health (MPAS 6947) |
| 1 month | Primary Care IV - Internal Medicine (MPAS 6974) |
| 1 month | Pediatric Critical and Acute Care Rotation - PCACLE Elective (MPAS 6913) |
| 1 month | Electives - Pediatric (MPAS 6936) or Adult (MPAS 6970) |
| 1 month | Vacation |
| ** Students must complete Outpatient and Inpatient Pediatric Medicine rotations prior to the Pediatric Critical and Acute Care Rotation. | |
Care of the Hospitalized Adult in a Novel Graduated Experience (Courses Are Subject to Change)
| Months | Type of Rotation |
| 1 month | Primary Care I - Ambulatory Pediatrics (MPAS 6930) |
| 1 month | Pediatric Specialty - Newborn Nursery (MPAS 6920) or Peds sub-specialty (MPAS 6936) or Adolescent Medicine (MPAS 6938) |
| 1 month | Inpatient Adult Medicine-CHANGE Track (MPAS 6944) |
| 1 month | Primary Care II - Family Medicine (MPAS 6940) |
| 1 month | Surgery - MPAS 6905 |
| 1 month | Emergency Medicine - MPAS 6948 |
| 1 month | Primary Care III - Women's Health (MPAS 6947) |
| 1 month | Primary Care IV - Internal Medicine (MPAS 6974) |
| 2 months | Electives - Pediatric (MPAS 6936) or Adult (MPAS 6970) |
| 1 month | Vacation |
Total credits vary based on track requirements.
* Subject to Change
Accreditation
The Accreditation Review Commission on Education for the Physician Assistant (ARC-PA) has granted Accreditation-Continued status to the Physician Assistant Program sponsored by the University of Colorado. Accreditation-Continued is an accreditation status granted when a currently accredited program is in compliance with the ARC-PA Standards.
Accreditation remains in effect until the program closes or withdraws from the accreditation process or until accreditation is withdrawn for failure to comply with the Standards. The approximate date for the next validation review of the program by the ARC-PA will be in 2026. The review date is contingent upon continued compliance with the Accreditation Standards and ARC-PA policy.