News & Patient Stories
Osseointegration/Limb Restoration News
-
How to Apply the Shrinker to Residual Limb after Primary or Revision AmputationOpens in a new window
Feb 19, 2025How to Apply the Shrinker to Residual Limb after Primary or Revision AmputationOpens in a new window Full story -
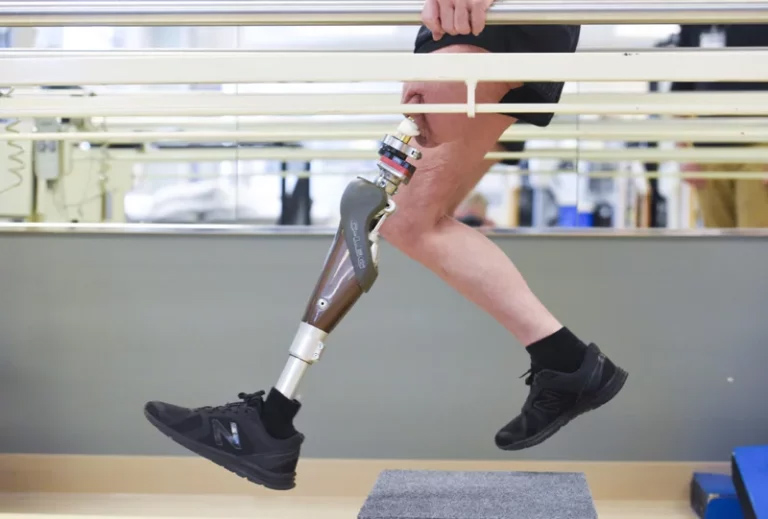
Innovative prosthetics center transforms care for amputeesOpens in a new window
Oct 26, 2024“When dealing with extremities at risk, there’s a subset of people for whom amputation becomes the right choice. That’s always been a pillar of the Limb Restoration Program,” said Dr. Jason Stoneback, an orthopedic traumatologist at UCHealth University of Colorado Hospital, who founded the program.Opens in a new window Full story -
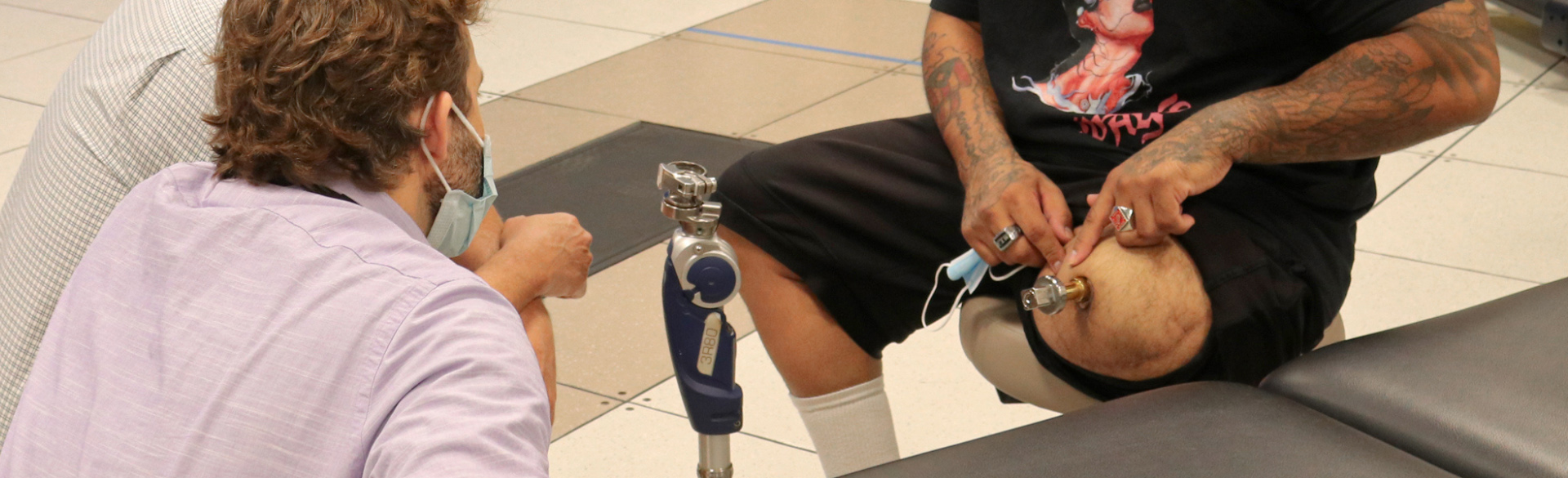
CU Program Transforms Care for Complex Limb InjuriesOpens in a new window
May 24, 2024The University of Colorado Limb Restoration Program is the first of its kind to deliver holistic, patient-centered care to people living with limb loss or who are at risk of losing a limb. Based at UCHealth University of Colorado Hospital on the CU Anschutz Medical Campus, the program provides comprehensive orthopedic, vascular, wound and rehabilitative care to a growing number of patients with complex extremity injuries.Opens in a new window Full story -
Beautiful Disaster | Hiba Azzam | UCHealth x Colorado Rockies
Dec 18, 2024"It's ok to grieve. It's ok to cry. Just don't get stuck there." UCHealth patient Hiba Azzam went from the ICU to throwing the first pitch at Coors Field with the Colorado Rockies.Full story
Trauma News
-
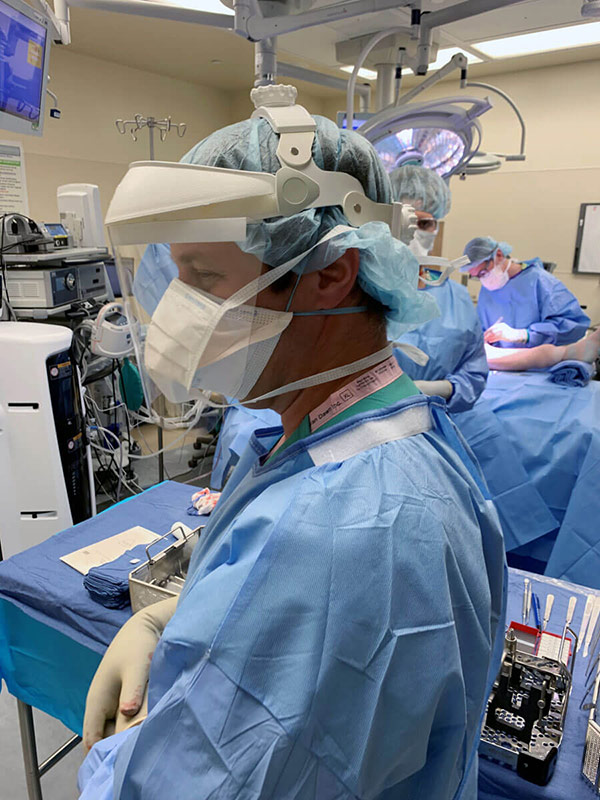
What if you break a hip (or leg, or whatever) during a pandemic?Opens in a new window
Apr 5, 2020What if you break a hip (or leg, or whatever) during a pandemic? People still get hurt. Orthopedic Trauma and other UCHealth trauma services have taken steps to be able to put patients back together and keep coronavirus out of the picture. By: Todd Neff, for UCHealthOpens in a new window Full story -

Tricky limb-restoration surgeries preserve Colten Fritzlan’s promising rodeo careerOpens in a new window
May 4, 2020Colten Fritzlan in action at the Tuff Hedeman Bull Riding Tour competition in El Paso, Texas on Feb. 8, 2020, after limb-restoration surgeries helped preserve his rodeo career. Photo courtesy Todd Brewer Photography.Opens in a new window Full story -
Stoneback JW
Sep 11, 2012What non-invasive methods can surgeons use to reliably differentiate between cellulitis and necrotizing fasciitis? What is the role of diagnostic imaging?: Advanced imaging has high sensitivity, specificity. Editorial. Orthopaedics TodayFull story