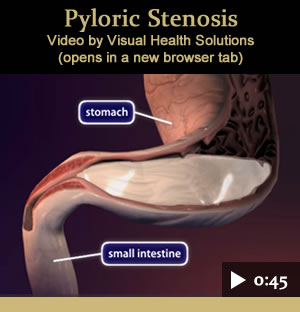
Hypertrophic Pyloric Stenosis
Pyloric stenosis, or narrowing of the outlet of the stomach, is a common cause of vomiting in early infancy. The vomit consists of undigested formula or breast milk and is caused by enlargement of the muscle that controls the flow of food from the stomach into the first part of the small bowel.
Pyloric stenosis is common, with an incidence of about 1 out of 500 live births. Pyloric stenosis is four times more common in males than females and tends to run in families.
How this Condition is Diagnosed
Infants who develop pyloric stenosis appear well during the first one or two weeks of life. Regurgitation or small spit-ups of formula or breast milk usually begins during the third to fifth week of life. These small spit-ups are followed by more frequent
episodes of vomiting, often prompting one or more visits to the pediatrician and formula changes. As the vomiting progresses over the next few days, it becomes more forceful and eventually projectile. The infant, however, remains hungry after vomiting
and otherwise appears well. If nothing is done, the infant will become dehydrated and lethargic.
The physical exam is often notable for a dry mouth and absence of tears when the infant cries. The diagnosis is usually made by ultrasound.
When ultrasonography is not available or if the pylorus is obscured by gas in the overlying bowel, an upper gastrointestinal (UGI) study should be performed. Positive findings on an UGI study include a narrow, elongated pyloric channel (string sign)
and indentation of the stomach by the enlarged pyloric muscle.
Infants with pyloric stenosis can develop abnormal electrolyte levels in their bloodstream and/or significant dehydration. Severely dehydrated infants should be given intravenous
fluids until their electrolyte disturbances have been sufficiently corrected to undergo an operation.
Treatment of Pyloric Stenosis
The standard operation for pyloric stenosis is division (cutting) of the enlarged pyloric muscle (called a pyloromyotomy). The operation is performed laparoscopically, or through a right upper-quadrant abdominal incision.
Once the pyloric muscle
is exposed, an incision is made along the length of the pyloric muscle. The pyloric muscle fibers are split apart, allowing the mucosal lining of the pyloric channel to bulge through the muscular defect, effectively opening up the channel and allowing
stomach contents to empty into the small bowel. Care must be taken to avoid entry into the stomach, pyloric channel, or small bowel.
Most infants are discharged home 24 to 48 hours after surgery.
This information is provided by the Department of Surgery at the University of Colorado School of Medicine. It is not intended to replace the medical advice of your doctor or healthcare provider. Please consult your healthcare provider for advice about a specific medical condition.